When a patient loses a tooth, the American Dental Association emphasizes that replacement is not just about appearance. It is about preventing the cascade of oral health problems that follow. Adjacent teeth shift, the jawbone deteriorates, and the chewing function diminishes. Yet despite dental implants being considered the gold standard for tooth replacement, a significant portion of patients either are not candidates for the procedure or choose different paths entirely.
The landscape of tooth replacement has evolved dramatically over the past decade. While implant technology continues to advance, so do options for dental implants and alternative solutions that address the varied needs, budgets, and medical situations of different patients. Some face bone loss that makes implants complex, others have medical conditions that complicate surgery, and many prefer less invasive options with lower upfront costs.
For anyone weighing their options after tooth loss, understanding the full spectrum of available treatments, from traditional bridges to modern mini-implants, can mean the difference between choosing based on assumptions and making an informed decision that aligns with their specific circumstances and long-term goals.
Why Patients Seek Alternatives to Traditional Dental Implants
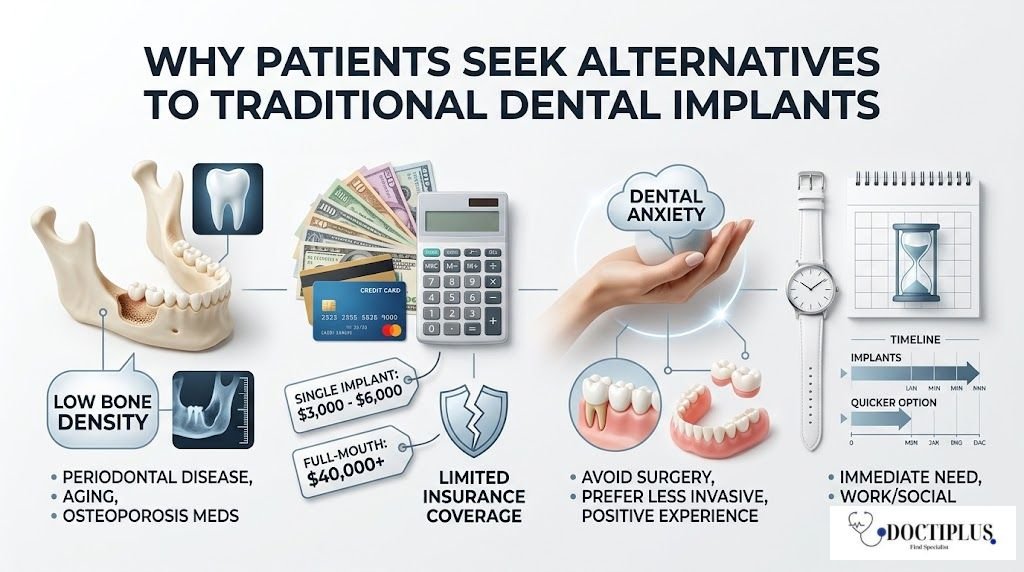
The reasons patients explore alternatives to traditional implants often stem from a complex interplay of medical, financial, and personal factors that are not immediately obvious. Bone density presents the most common clinical barrier. Implants require sufficient jawbone to anchor properly, but many patients have experienced bone loss from prolonged tooth absence, periodontal disease, or natural aging. While bone grafting can address this issue, it adds months to treatment time and substantial cost.
Medical conditions create another significant hurdle. Patients with uncontrolled diabetesface higher implant failure rates due to impaired healing, while those taking certain medications like bisphosphonates for osteoporosis may be at risk for complications. Cancer patients who have undergone head and neck radiation often lack the healthy tissue needed for successful osseointegration, the process by which bone grows around and bonds with the implant.
| Aspect | Details |
|---|---|
| Key Factor | Financial considerations play a major role, especially when insurance coverage is limited |
| Cost of Single Implant | $3,000 – $6,000 per tooth |
| Cost of Full-Mouth Implants | Can reach $40,000 or more |
| Budget Concern | High costs make implants less accessible for many patients |
| Alternative Options | Partial dentures and dental bridges |
| Benefit of Alternatives | Provide functional tooth replacement at a much lower cost |
Some patients prefer to avoid surgery entirely, whether due to anxiety, previous negative experiences, or philosophical preferences for less invasive treatments. Others face timing constraints, needing immediate tooth replacement for work or social obligations that cannot accommodate the months-long implant process.
How Dental Implants Work and What Influences Their Success
Understanding implant mechanics helps clarify why alternatives exist and when they might be preferable. Dental implants function by replacing the entire tooth structure, both crown and root. A titanium post is surgically placed into the jawbone, where it undergoes osseointegration, a biological process in which living bone tissue grows around and fuses with the implant surface over 3 to 6 months.
This integration creates remarkable stability. Unlike natural teeth, which are held in place by periodontal ligaments that allow slight movement, properly integrated implants become essentially part of the jawbone. They can withstand normal chewing forces and often last decades with proper care.
However, this very strength reveals why implants are not universal solutions. Osseointegration requires specific conditions: adequate bone density, a healthy blood supply, the absence of infection, and a proper healing response. Patients who smoke face significantly higher failure rates because nicotine restricts blood flow to healing tissues.
Success also depends heavily on maintaining oral hygiene. While implants cannot decay, they can develop peri-implantitis, a destructive inflammatory condition similar to severe gum disease that can cause implant failure. This condition affects an estimated 20 to 30 percent of patients with implants, according to periodontal research, making alternatives attractive for patients with poor oral hygiene habits or limited ability to maintain complex cleaning routines.
Main Alternatives to Traditional Dental Implants
The landscape of implant alternatives has expanded significantly, offering both fixed and removable solutions that address different clinical scenarios and patient preferences. Modern alternatives range from minimally invasive procedures to comprehensive restorations, each with distinct advantages depending on the specific situation.
Fixed Alternatives: Bridges and Resin-Bonded Options
Traditional bridges remain the most common fixed alternative to single implants. A bridge uses adjacent teeth as anchors, with crowns placed on these abutment teeth connected to a replacement crown that spans the gap. The process requires reshaping the neighboring teeth to accommodate crowns, but it avoids surgery entirely and can be completed in two to three weeks.
Implant-supported bridges offer a hybrid approach for multiple missing teeth. Instead of using natural teeth as anchors, two to four implants support a bridge spanning several teeth. This option requires fewer implants than replacing each tooth individually, reducing cost and surgical complexity while still providing a fixed, stable restoration.
Resin-bonded bridges, also called Maryland bridges, present the most conservative fixed option. These bridges attach to the back surfaces of adjacent teeth with metal or ceramic wings, requiring minimal tooth preparation. They work best for front teeth with light bite forces and offer an excellent temporary solution while planning more definitive treatment. However, they are less durable than traditional bridges and may debond over time.
Removable Alternatives: Dentures and Mini Implants
Partial dentures use clasps or precision attachments to connect to remaining teeth, replacing multiple missing teeth with a removable appliance. Modern partials can be nearly invisible when designed properly and cost significantly less than multiple implants or bridges.
Complete dentures replace entire arches of teeth and rely on suction, adhesives, and muscle control for retention. While traditional dentures have limitations in chewing efficiency and retention, advances in materials and techniques have significantly improved comfort and function.
Snap-on dentures represent a hybrid solution, using two to four implants with special attachments that allow dentures to click securely in place while remaining removable for cleaning. This approach provides dramatically improved stability compared to conventional dentures at a fraction of the cost of full implant restoration.
Mini dental implants offer another alternative, using smaller-diameter implants that require less bone and can often be placed without surgery. While not as strong as traditional implants, they are suitable for denture stabilization or single tooth replacement in areas with limited space or bone.
Advantages and Disadvantages of Dental Implant Alternatives
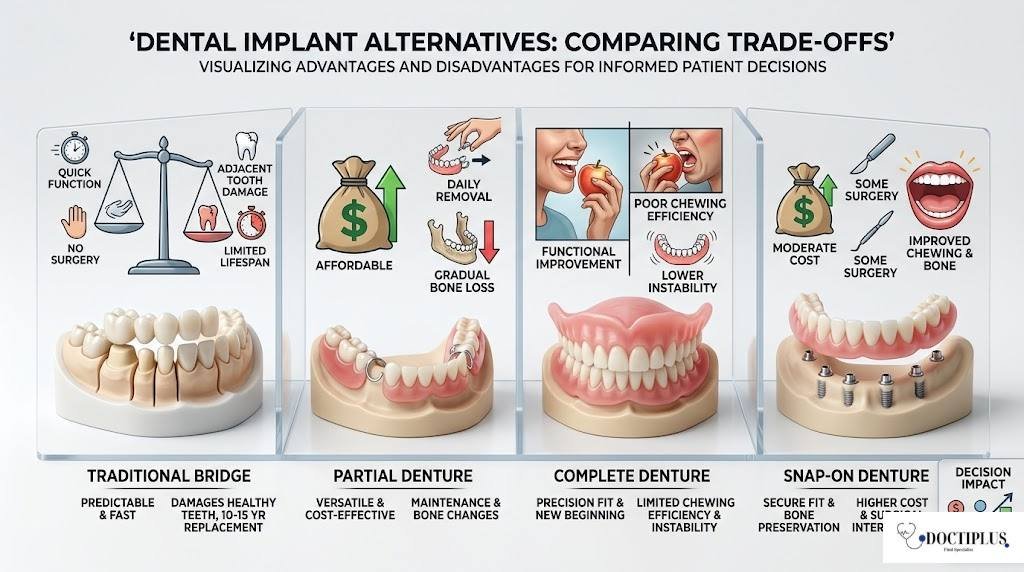
Each alternative presents distinct trade-offs that matter differently depending on patient priorities, oral health status, and long-term goals. Understanding these trade-offs helps clarify when alternatives are superior to implants for specific situations.
Traditional bridges excel in predictability and speed. They have been refined over decades and can restore normal chewing function and appearance quickly without surgery. However, they require the removal of healthy tooth structure from adjacent teeth, potentially shortening their lifespan. Bridges typically last 10 to 15 years before requiring replacement, and if the anchor teeth develop problems, the entire restoration fails.
Partial dentures offer excellent versatility and affordability. They can replace multiple teeth anywhere in the mouth and can be adjusted as oral conditions change. Modern materials create nearly invisible clasps and a comfortable fit. The primary disadvantages include daily removal for cleaning, potential food trapping, and gradual bone loss under the denture base since they do not stimulate bone like implants.
Complete dentures provide dramatic functional improvement for patients missing all teeth, primarily when properly designed and fitted. Modern techniques such as digital impressions and CAD/CAM manufacturing have significantly improved precision. However, dentures typically achieve only 20 to 30 percent of normal chewing efficiency, and lower dentures, especially, can be unstable without implant support.
Snap-on dentures bridge the gap between conventional dentures and full implant restoration. They provide 70 to 80 percent of normal chewing function while remaining removable for easy cleaning. The implant component helps preserve bone and dramatically improves retention. The main limitations include a higher cost than conventional dentures and the need for some surgical intervention.
| Aspect | Details |
|---|---|
| Key Factor | Cost varies by region and treatment complexity |
| Cost of Alternatives | $500 (simple partial dentures) to $15,000 (implant-supported bridges) |
| Cost of Full Implant Treatment | $20,000 – $40,000 for comprehensive care |
| Affordability Insight | Alternatives are generally more budget-friendly than full implant solutions |
| Decision Impact | Patients often choose based on cost, needs, and treatment goals |
How to Choose the Right Tooth Replacement Option for Your Needs
The decision between implants and alternatives should be based on a comprehensive evaluation of multiple factors that extend far beyond initial cost or convenience. Bone quality and quantity often dictate feasibility. Patients with significant bone loss may find alternatives more practical than extensive grafting procedures.
Overall health status plays a crucial role in treatment selection. Patients with well-controlled medical conditions often make excellent implant candidates, while those with compromised immune systems, bleeding disorders, or medications that affect healing may benefit from less invasive alternatives. Age itself is not a barrier, but physiological age and healing capacity matter more than chronological age.
Oral hygiene capability significantly influences long-term success regardless of treatment choice. Patients who struggle with effective plaque control may achieve better outcomes with removable options that can be cleaned thoroughly outside the mouth. Conversely, patients with excellent hygiene often prefer fixed solutions that feel and function like natural teeth.
Financial planning should consider total lifetime costs, not just initial treatment fees. While implants cost more upfront, their longevity often makes them economical over the long term. Alternatives may require periodic replacement or adjustment, creating ongoing expenses that accumulate over time.
The most successful treatment decisions involve honest discussion about expectations, limitations, and long-term goals. Patients who understand the trade-offs of their chosen treatment typically experience higher satisfaction regardless of which option they select. Rather than viewing alternatives as compromises, informed patients often discover that the best treatment is the one that best fits their individual circumstances and priorities.
Conclusion
Choosing the right tooth replacement solution is a deeply personal decision that depends on your unique oral health, medical history, budget, and lifestyle. Dental implants remain the gold standard for durability and function, but they are not the right choice for every patient. Fixed bridges, partial dentures, complete dentures, snap-on dentures, and mini implants each offer meaningful benefits under the right circumstances. The best path forward begins with an honest conversation with a qualified dental professional who can assess your bone density, overall health, and long-term goals. Armed with accurate information and realistic expectations, every patient can find a tooth replacement solution that restores both confidence and quality of life.
Disclaimer
This article is intended for general informational purposes only and does not constitute medical or dental advice. The content should not be used as a substitute for professional diagnosis, treatment recommendations, or consultation with a licensed dentist or oral health specialist. Individual treatment needs vary, and only a qualified dental professional can assess whether a specific procedure is appropriate for your oral health situation. Always consult your dentist or a dental specialist before making any decisions regarding tooth replacement or dental treatment.
References
- American Dental Association. Tooth Replacement Options. ADA.org.
- Academy of Osseointegration. What Are Dental Implants? Academy of Osseointegration.
- Derks J, Tomasi C. Peri-implant health and disease: a systematic review of current epidemiology. Journal of Clinical Periodontology. 2015.
- National Institute of Dental and Craniofacial Research. Dental Implants. NIDCR.NIH.gov.
- American Academy of Periodontology. Bone Grafting for Dental Implants. Perio.org.
- Felton DA. Complete Edentulism and Comorbid Diseases: An Update. Journal of Prosthodontics. 2016.

