Dog bites don’t usually feel like something you need to prepare for, that is, until they happen. Then suddenly you’re standing there, a bit shaken, looking at a wound and wondering if it’s serious or not.
A lot of people assume a bite is only a problem if it looks bad right away and if there’s a deep cut, heavy bleeding, or obvious damage. But that’s not really how it works. Some of the more dangerous issues, like infection, swelling and pain that wasn’t there at first, show up later.
In the U.S., around 4.5 million dog attacks that result in bites happen every year, and roughly 1 in 5 of those end up needing medical care. And in Arizona, with how many people spend time outdoors or around pets, the chances aren’t exactly low either.
So it helps to know what to do. What actually matters in those first few minutes, and what can wait. Not in theory, but in real terms.
Why Dog Bites Can Turn Serious Quickly
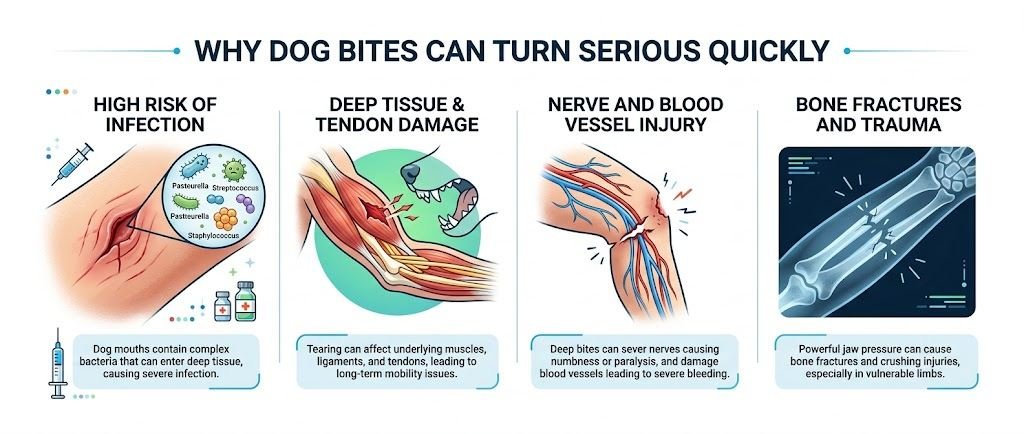
At a glance, a bite might not look like a big deal, especially if it’s a small puncture or a shallow break in the skin. But the size of the wound doesn’t always match the risk.
Dogs carry bacteria in their mouths, and the problem starts when that bacteria gets pushed under your skin. Some of the more common ones, like Pasteurella, can cause infections pretty fast.
About 10% to 20% of wounds get infected. That number goes up for certain areas of the body. Hands are a big one, fingers too, because there’s less tissue there, and bacteria can settle in deeper.
Puncture wounds are tricky. They look small, but they seal over quickly, which can trap bacteria inside, and you don’t see what’s going on underneath.
Arizona is a desert state, and there’s heat, sweat, and a lot of dust. All of that can affect how a wound behaves after the fact. If it’s not cleaned properly, things can shift in the wrong direction within a day or two.
That delay is usually where people get caught off guard.
What to Do Right After an Attack
The first few minutes are the most important. You don’t need to panic, but you do need to act.
The first step is simple. Get away from the dog and create some distance so nothing escalates. Then take a look at the wound and if it’s bleeding, apply pressure. Put a clean cloth or a gauze over it until the bleeding slows down.
After that, rinse the wound. Running water is key here, so be sure to let it flow over the area for a few minutes. Then wash it with soap, but not aggressively. You’re not scrubbing a stain out of fabric. Just clean it well enough to reduce what’s sitting on the surface. Five minutes of rinsing is a good baseline. Longer if the wound is deeper or dirt got into it. Once that’s done, cover it with something clean, like a sterile bandage if you have one. If not, anything clean is better than leaving it exposed.
A couple of things people still do that aren’t helpful, like pouring strong chemicals into the wound. Repeated use of hydrogen peroxide, for example, can actually slow healing because it damages healthy tissue along with bacteria. Another one is trying to close the wound at home. That can trap bacteria inside and make things worse later.
Cleaning it is step one, not the final step.
When You Should Get Medical Help
Some bites clearly need medical attention, while others sit in that gray area where people hesitate.
If the wound is deep or still bleeding after about 10 minutes of steady pressure, that’s a clear sign to go in. Bites on the face, hands, feet, or near joints should also be checked. These areas are more sensitive, and complications show up faster.
Then some signs develop later, such as redness that spreads, swelling that keeps getting worse, warmth around the wound, pus and increasing pain instead of less. Fever is another signal. Not always immediate, but if it shows up, it matters.
Children fall into a higher-risk group. About half of all dog bite injuries in the U.S. involve kids. And the injuries tend to be more severe, often around the head or neck. People with weaker immune systems need to be more careful, too. Even a smaller bite can escalate faster in those cases.
If you’re unsure, getting it checked is usually the safer move. Urgent care can handle many situations; more serious injuries go straight to the ER.
What Happens When You Go In
Once you’re in a clinic or hospital, the approach is pretty straightforward. They’ll clean the wound again, usually more thoroughly than what you can do at home, and sometimes that includes removing damaged tissue. It sounds intense, but it helps prevent infection.
Not every wound gets stitches. In fact, many don’t, especially if there’s a higher risk of infection. Leaving it open allows it to drain and heal more safely. Antibiotics come into play depending on the wound. High-risk areas, deeper bites, or signs of early infection usually mean a prescription.
Tetanus shots are often updated if needed. And if there’s any question about the dog’s vaccination status, they’ll evaluate rabies risk. Rabies is rare in the U.S., but when it comes to that, doctors don’t take chances.
After that, you’ll get instructions for care at home. And you should follow them.
Dealing With the Aftermath and the Costs
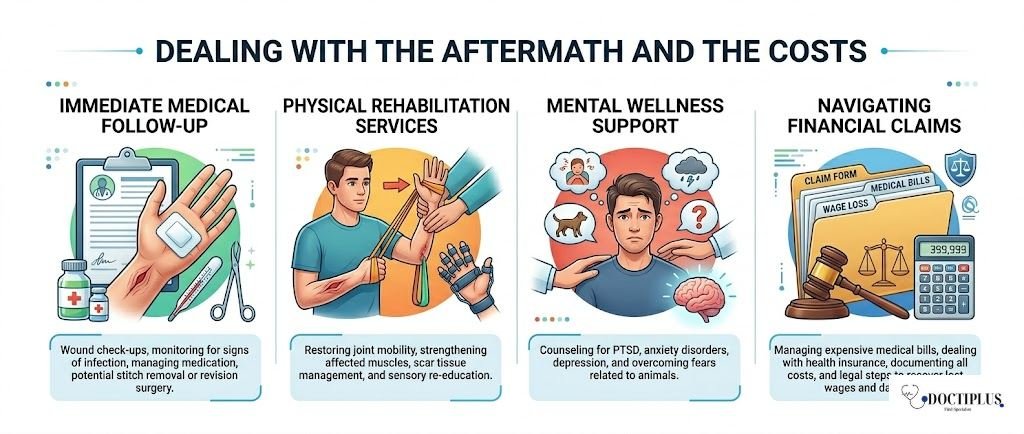
This is the part that doesn’t get talked about much at the start. You go in, get treated, maybe get antibiotics, and head home. But recovery isn’t always one visit; there can be follow-ups and referrals if the injury is more complex.
Emergency visits, medications, and time off work can cost a lot. In situations where the bite involves someone else’s dog, some people look into what their options are for handling those costs. That might include consulting with a Mesa dog bite lawyer to understand what’s possible in their specific case.
Not everyone goes that route, however, and it’s not something you need to think about right away. But when medical bills start stacking up, it becomes part of the bigger picture.
The main focus stays on healing, but it helps to know there are options if things get complicated.
Taking Care of the Wound at Home
Once you’re back home, the routine is simple, but it needs to be consistent. Keep the wound clean, change the dressing as instructed, and be sure to wash your hands before touching it. That alone prevents a lot of problems.
Try not to mess with it too much. No picking, no unnecessary contact. Watch how it changes over time. A little redness at first can be normal. What you’re looking for is progression. Is it spreading? Getting more painful? Starting to drain? Those are signs to get it looked at again.
If you were given antibiotics, take the full course even if things look better halfway through. Stopping early can allow bacteria to come back.
It’s basic care, but skipping steps is where complications start.
Final Thoughts
Dog bites aren’t something you plan for, but knowing what to do changes how things play out.
Clean the wound properly and don’t assume it’s minor just because it looks that way. Pay attention to how it changes over time. Around 1 in 5 bites ends up needing medical care. That’s enough to take it seriously without overthinking every situation.
Living in Arizona means being around dogs is part of daily life. Most of the time, there’s no issue, but when something does happen, a clear head and a few practical steps go a long way.
Disclaimer
This article is intended for informational purposes only and does not constitute medical or legal advice. While it provides general guidance on handling dog bite injuries, individual cases can vary significantly. Dog bites may lead to serious infections or complications that require professional evaluation. If you experience a bite, especially one that is deep, bleeding heavily, or showing signs of infection, seek immediate medical attention from a qualified healthcare provider.
Additionally, any mention of legal options is for general awareness only and should not be considered legal counsel. For specific concerns regarding liability or compensation, consult a licensed attorney in your area. Always rely on qualified medical and legal professionals for advice tailored to your situation.
References
- Brook, I. (2009). Management of human and animal bite wounds. Journal of Clinical Microbiology. DOI: 10.1128/JCM.01200-09
- Goldstein, E. J. C. (1998). Bite wounds and infection. Clinical Infectious Diseases. DOI: 10.1086/514299
- Medeiros, I., & Saconato, H. (2001). Antibiotic prophylaxis for mammalian bites. Cochrane Database of Systematic Reviews. DOI: 10.1002/14651858.CD001738
- Chen, E., Hornig, S., Shepherd, S. M., Hollander, J. E. (2000). Primary closure of mammalian bites. Academic Emergency Medicine. DOI: 10.1111/j.1553-2712.2000.tb02071.x
- Callaham, M. (1980). Prophylactic antibiotics in dog bite wounds. Annals of Emergency Medicine. DOI: 10.1016/S0196-0644(80)80020-5
- Morgan, M., & Palmer, J. (2007). Dog bites. BMJ. DOI: 10.1136/bmj. 39105.659919.BE
- Centers for Disease Control and Prevention (CDC). (2020). Rabies prevention and control. Morbidity and Mortality Weekly Report. DOI: 10.15585/mmwr.rr6902a1
- World Health Organization (WHO). (2018). Rabies epidemiology and prevention. DOI: 10.2471/BLT.17.204586

