Hospitals and public health departments both work to keep people healthy, but they do it in different ways. Hospitals focus on treating people who are already sick or injured. Doctors, nurses, and other medical staff diagnose illnesses, provide treatment, and help patients recover.
Public health departments, on the other hand, focus on preventing illness before it happens. They study health trends in communities, organize vaccination programs, promote healthy habits, and work to prevent the spread of disease.
Even though their roles differ, both systems are important to a strong healthcare system. Hospitals care for individuals when they need medical treatment, while public health departments help the public.
Two Systems, One Goal
Hospitals and public health departments both exist to protect and improve human health, yet the way they pursue that goal looks almost nothing alike. Walking into a hospital, you encounter nurses monitoring vital signs, physicians reviewing imaging results, and pharmacists filling prescriptions. Walking into a public health department, you are more likely to find epidemiologists analyzing disease trends, community health workers designing vaccination outreach, and policy analysts studying the social conditions that make certain neighborhoods sicker than others.
Both systems are essential. Neither can fully substitute for the other. Understanding how they differ helps patients make better decisions about where to seek care, helps students choose the right educational path, and helps communities advocate more effectively for their health needs.
Key point for patients: Hospitals treat you when you are sick or injured. Public health departments work to prevent illness before it reaches you. Both systems are part of your healthcare, even if you only notice one of them when something goes wrong.
Fundamental Difference: Individual Care vs. Population Health
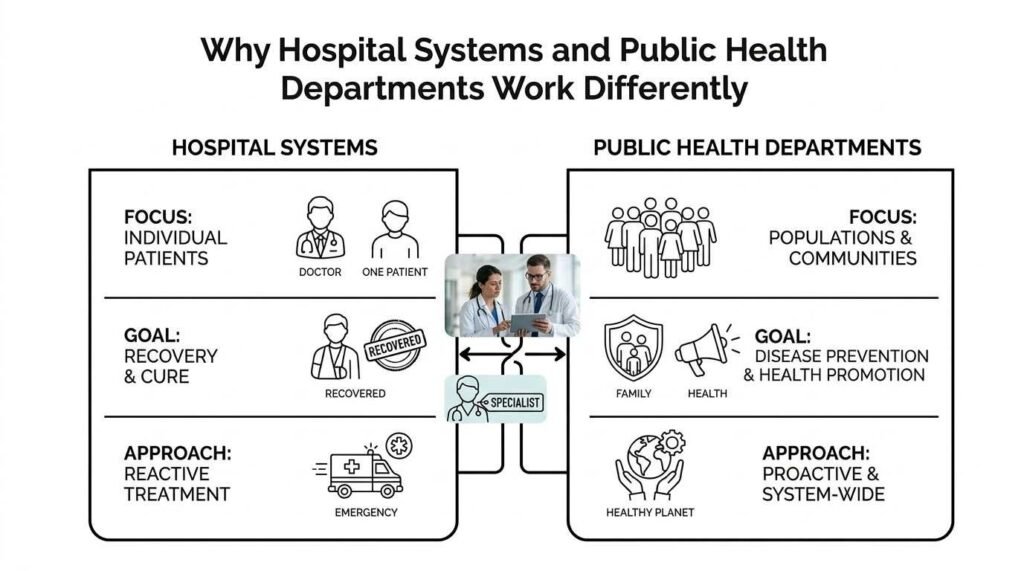
What hospitals focus on
Hospital care centers on the individual patient. When you arrive at a hospital, the entire system orients itself around your specific symptoms, history, and needs. Physicians examine you, develop a treatment plan, and track your recovery. Nurses monitor your condition around the clock. Every decision, from which medication to prescribe to when to discharge you, is shaped by what is best for you as an individual.
Hospital activity moves quickly because patient conditions can change within minutes. Emergency departments stabilize injuries in real time. Intensive care units continuously monitor life-threatening conditions. Operating rooms respond to surgical emergencies on short notice. Speed, precision, and coordination are built into the culture of hospital care because individual lives depend on them.
What public health departments focus on
Public health departments examine health at a much larger scale. Their concern is not what is happening to one patient in one room, but what is happening across thousands of households in a city, county, or region. A rise in respiratory illness in a particular neighborhood, a decline in childhood vaccination rates at a cluster of schools, or an unusual pattern of food-borne illness across a county are exactly the kinds of signals that public health professionals are trained to detect and investigate.
Rather than treating illness one person at a time, public health teams organize responses that reach large groups simultaneously. A vaccination drive, a school-based mental health program, or an environmental inspection of water quality serves entire communities with a single coordinated effort.
Why this matters for you: When your local public health department runs a free flu vaccination clinic or issues a drinking water advisory, that is population-level healthcare working directly in your life. These services often operate quietly in the background, which is why their value is easy to overlook until a crisis makes it visible.
Educational Paths: Choosing the Right Degree
Career preparation for both sectors begins with education, and the programs reflect the very different work professionals will face. Understanding the distinction between degree options is important for students deciding on a career direction.
Hospital and health system administration
Hospital leadership roles typically attract individuals trained in healthcare administration, hospital finance, operations management, and regulatory compliance. Working within large medical systems requires familiarity with clinical workflows, insurance structures, patient services billing, and the complex logistical demands of operating facilities that operate 24/7. Common credentials include a Master of Health Administration (MHA) or a Master of Business Administration with a healthcare concentration.
Public health careers
Public health education follows a different path. Programs in epidemiology, community health planning, environmental health, and health policy prepare graduates to examine trends affecting entire populations. Questions about MHA vs MPH degree options frequently arise for students entering this field, as each degree offers distinct career opportunities. A Master of Health Administration prepares professionals to manage healthcare organizations and hospital systems, with a focus on operations, finance, and leadership. A Master of Public Health prepares graduates to address disease patterns, design prevention programs, and lead population health research. The decision often comes down to whether a student wants to work inside a clinical system or across the broader landscape of community and population health.
Guidance for students: If you are drawn to managing hospitals, improving clinical operations, or working in healthcare finance, an MHA is likely the stronger fit. If you are drawn to epidemiology, disease prevention, environmental health, or health policy, an MPH will better prepare you for that work. Many professionals eventually pursue both.
How Decisions Are Made in Each System
Hospital decision-making
Decision-making inside hospital networks follows a structured chain of leadership. Executive teams establish long-term strategies related to facility growth, service lines, and financial sustainability. Department directors coordinate clinical operations, staffing, and service delivery within specialized units such as surgery, emergency care, and oncology. Many decisions are driven by operational performance metrics, patient safety standards, and regulatory compliance requirements tied to accreditation bodies such as The Joint Commission.
Clinical decisions at the bedside are made by physicians, nurses, and interdisciplinary teams based on patient-specific data, established treatment protocols, and real-time clinical judgment. Speed and clarity of communication are essential because errors in clinical environments can have immediate consequences.
Public health decision-making
Government health agencies operate within a distinct framework shaped by public administration and policy. Programs and interventions may require coordination with municipal leaders, state authorities, elected officials, and public advisory boards before moving forward. Health commissioners, epidemiologists, and program managers regularly collaborate with community organizations, schools, faith communities, and nonprofit groups while developing initiatives that must work across diverse populations.
This process moves more slowly by design. Public health interventions that affect entire communities carry significant social and political dimensions, and broad input tends to produce more equitable and effective outcomes.
What Staff Actually Do Day to Day
Inside a hospital
Hospital operations revolve around the steady movement of patients through clinical spaces. Medical teams evaluate symptoms, perform procedures, monitor recovery, and coordinate follow-up care. Administrative teams manage scheduling systems, insurance documentation, medical records, and facility operations. Communication across departments is continuous because treatment decisions often depend on coordinated input from physicians, nurses, technicians, and pharmacists working simultaneously.
• Clinical staff: Physicians, nurses, surgical teams, therapists, pharmacists, radiologists
• Administrative staff: Medical records, billing, scheduling, compliance, quality improvement
• Support staff: Environmental services, patient transport, nutrition, security
Inside a public health department
Public health work unfolds across a much wider geographic and social landscape. On any given day, staff might be analyzing disease surveillance reports, coordinating a school-based vaccination drive, inspecting restaurant kitchens, conducting environmental sampling near an industrial site, or presenting health data to city council members.
• Epidemiologists: Track disease trends, investigate outbreaks, analyze population health data
• Community health workers: Deliver education, conduct outreach, build trust with underserved communities
• Environmental health specialists: Monitor air, water, and food safety; enforce health codes
• Health policy analysts: Develop and evaluate programs, advise government officials, write legislation
How Each System Collects and Uses Data

Patient-level data in hospitals
Hospitals gather highly detailed information during diagnosis and treatment. Electronic health records capture laboratory results, imaging reports, medication histories, physician observations, and nursing assessments. This data allows clinicians to monitor individual health progress and coordinate care across departments. Hospital administrators use aggregated patient data to evaluate service quality, clinical outcomes, and operational efficiency.
Population-level data in public health
Public health departments collect information through surveillance systems designed to detect patterns across large populations. Epidemiologists examine case reports submitted by hospitals and clinics, monitor vaccination rates, and analyze trends across geographic regions. Data sources include health surveys, environmental monitoring programs, school health records, vital statistics registries, and national disease reporting systems such as those maintained by the Centers for Disease Control and Prevention (CDC).
For patients: The data your hospital collects about your individual care eventually contributes to population-level insights. De-identified patient data from hospital feeds into the surveillance systems that public health departments use to detect disease outbreaks and track treatment effectiveness across communities.
How Resources Are Allocated
Hospital budgets
Hospital budgets are built around maintaining clinical services and facility operations. Major cost categories include medical equipment and diagnostic technology, clinical staff salaries, pharmaceutical supplies, building infrastructure, and information technology systems. Departments such as surgery, emergency care, and intensive care require advanced equipment and highly specialized personnel, resulting in substantial operational costs. Administrators continuously evaluate patient demand, service capacity, and financial sustainability.
Public health budgets
Public health departments direct funding toward programs designed for community-wide impact. Budgets support vaccination campaigns, disease surveillance infrastructure, health education initiatives, environmental health inspections, and maternal and child health programs. A significant portion of public health funding comes from federal and state government allocations, and many programs depend on competitive grants that require ongoing renewal.
Resource planning in public health often involves formal partnerships with schools, nonprofit organizations, and local governments because programs routinely reach people outside of healthcare facilities. The return on investment for public health spending is well documented. Research consistently shows that every dollar spent on prevention generates several dollars in avoided treatment costs.
Geographic Scope of Services
How hospitals serve their communities
Hospitals typically serve patients who travel to their facilities or belong to a connected network of clinics and medical centers. A large hospital system may operate multiple campuses and partner facilities across a metropolitan area, but services remain anchored to physical locations where patients receive direct care. Access depends significantly on proximity, transportation, insurance coverage, and the availability of specialist services at a given campus.
How public health departments cover their jurisdictions
Public health departments are responsible for the health of everyone living within a defined geographic area, whether or not they ever set foot in a healthcare facility. Their jurisdiction may cover a city, a county, or an entire state. Programs are designed to reach residents through community centers, schools, mobile health units, social media campaigns, and direct field investigations. Coverage is not limited by physical infrastructure because the mission extends to every household in the jurisdiction.
Research Priorities in Each System
Clinical research in hospitals
Clinical trials and hospital-based research focus primarily on improving treatments and patient outcomes. Physicians and medical researchers study new therapies, surgical techniques, medical devices, and pharmaceutical interventions. Results from clinical studies influence medical guidelines, shape prescribing practices, and expand the range of treatment options available to future patients. If you are a patient interested in participating in a clinical trial, your physician or a hospital research coordinator can explain eligibility and what participation involves.
Population health research in public health
Public health research addresses questions at the community and societal level. Epidemiologists analyze patterns of disease spread, the influence of environmental conditions on health outcomes, and the effectiveness of prevention programs at scale. Researchers examine large population datasets to understand how income, housing, access to healthy food, social connections, and environmental exposure shape community health. Findings from this research guide policy decisions, inform allocation of public health funding, and drive large-scale prevention strategies.
For patients interested in research: If you want to know whether a clinical trial is available for a condition you or a family member is managing, the U.S. National Library of Medicine maintains a searchable database of active trials at clinicaltrials.gov. Participation is always voluntary and requires informed consent.
How Hospitals and Public Health Departments Collaborate
Despite their structural differences, hospitals and public health departments depend on each other. Hospitals are required to report certain diagnoses, including confirmed cases of tuberculosis, measles, hepatitis, and foodborne illness, to public health authorities. These reports feed the surveillance systems that allow public health teams to detect outbreaks early and coordinate responses before they spread further.
During public health emergencies such as influenza pandemics, natural disasters, or disease outbreaks, hospitals and public health departments coordinate closely on patient surge management, resource sharing, and public communication. The COVID-19 pandemic made this interdependence visible to millions of people who had never before considered how the two systems fit together.
Community benefit programs operated by nonprofit hospitals also blur the line between individual and population health. Many hospital systems fund community health needs assessments, support mobile health clinics, and partner with public health departments on chronic disease prevention initiatives that extend well beyond their patient populations.
What This Means for You
Understanding the difference between hospital systems and public health departments helps you navigate healthcare more effectively. When you need diagnosis, treatment, or emergency care, a hospital is the right place to turn. When you want to understand disease risks in your community, access free prevention services, or advocate for healthier conditions in your neighborhood, public health departments are the relevant resource.
Both systems benefit from informed, engaged communities. Patients who understand what each system does are better positioned to ask the right questions, use available services, and participate in the policy conversations that shape healthcare for everyone.
Disclaimer
This article is provided for general informational and educational purposes only. It does not constitute medical, legal, or professional career advice. It should not be used as a substitute for consultation with a licensed healthcare provider, academic advisor, or qualified public health professional. Healthcare system structures, funding mechanisms, scope-of-practice regulations, and educational program requirements vary significantly by state and institution and are subject to change. Statistics and descriptions reflect information available at the time of writing. Always verify current information with the relevant licensing body, institution, or government agency.
References and Resources
- Centers for Disease Control and Prevention (CDC). Public Health 101 Series. https://www.cdc.gov/training/publichealth101
- U.S. Department of Health and Human Services. About the U.S. Public Health System. https://www.hhs.gov/ash/index.html
- National Association of County and City Health Officials (NACCHO). Local Health Department Resources. https://www.naccho.org
- Association of State and Territorial Health Officials (ASTHO). State Public Health Resources. https://www.astho.org

