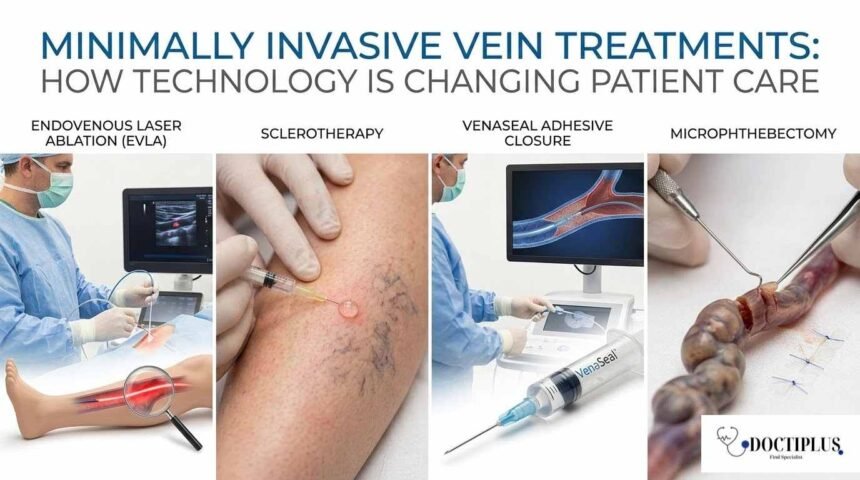
Hundreds of millions of dollars are spent to treat vein-related conditions, and the most common symptoms are varicose veins or chronic venous insufficiency. High blood pressure in the veins and swollen varicosities were once thought of as either a cosmetic annoyance or a disease that needed invasive procedures, but vein disease is viewed very differently today. Innovations in medical technology are changing how physicians diagnose, manage and treat vascular conditions with minimally invasive methods. These innovations have also improved the patient experience as well as clinical outcomes.
Modern vein care is all about precision, efficiency and comfort. Patients today can benefit from effective treatments with minimal time away from their regular activities, rather than the protracted, invasive surgical procedures and lengthy hospital stays of the past. This shift is part of a wider trend in healthcare, which now strives to provide targeted and more personalized care that disrupts people’s lives less with the help of technology.
Familiarity with how these innovations are influencing vein therapy can empower patients of all ages and demographics to make informed choices, while also illustrating the increasing influence of innovation on vascular well-being.
What Is Vein Disease and Why Is It Challenging?
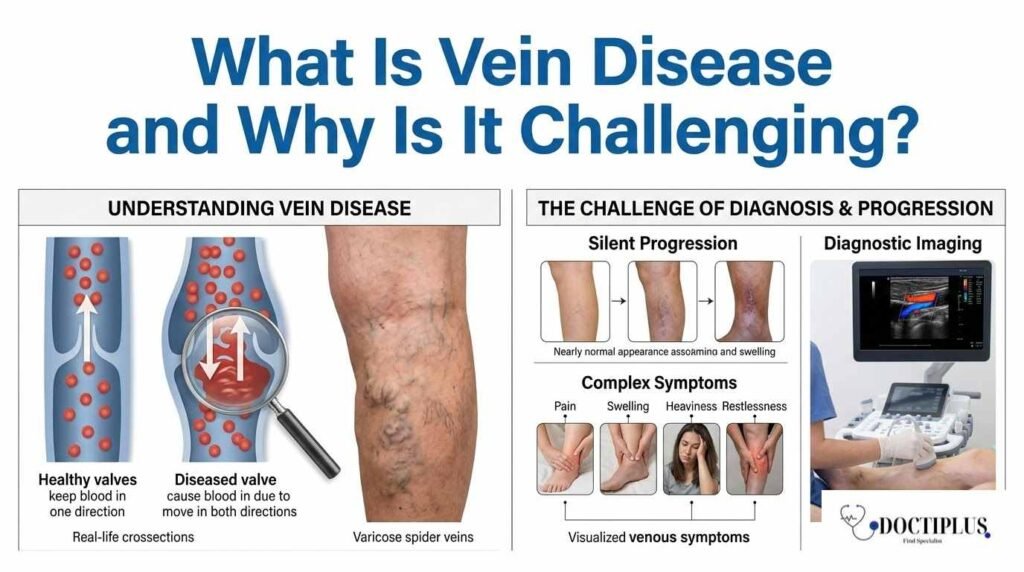
After veins have delivered oxygen and nutrients to all tissues, they take blood back to the heart, an important thing. In the legs, this process is especially difficult because blood must be transported up against gravity. Veins prevent blood from flowing backward at these low pressures by using one-way valves to facilitate this movement.
When these valves become weaker or fail, blood can slow down and pool in the veins, meaning there is higher pressure against the wall of that vessel, and it ends up stretching. This condition results in varicose veins, which are most recognizable as swollen, bulging veins that appear under the skin. Some might only have cosmetic complaints, whereas others suffer from pain, swelling, heaviness, itching and tiredness of the legs.
Untreated vein disease can descend into chronic venous insufficiency, a serious condition that can lead to changes in the skin and inflammation, even ulcers. These complications underscore the need for early diagnosis and treatment.
Traditionally, treating these conditions included surgical vein stripping, a process that surgically removed the affected vein through incisions. Although effective, it came with considerable pain and recovery time. Technology has evolved and allowed for less invasive and more patient-friendly solutions in today’s world.
Emerging Popularity of Less-Intense Treatments
These procedures usually use small catheters, ultrasound guidance and focused energy or medication to close or seal the dysfunctional vein.
These procedures do not remove the vein but reroute blood flow to more healthy vessels. Once the injured, malfunctioning vein closes, the blood flow is redirected in natural ways that improve overall circulation and relieve symptoms.
Another major benefit of minimally invasive treatments is that they can be done with local anesthesia. Patients are awake and comfortable during the procedure, and most treatments take less than an hour to complete. Recovery is typically rapid, so people are able to resume normal activities soon after treatment.
With these advantages, minimally invasive procedures have become a preferred option for patients and healthcare providers alike.
Advanced Imaging and Precision Diagnosis
High-resolution imaging techniques have changed the game in vein care. Duplex ultrasound is the diagnostic gold standard for vein disorders. This non-invasive imaging technique enables physicians to visualize blood flow inside the veins and locate sites where valves do not function properly.
Proper treatment hinges on accurate diagnosis. With the precise location of where the problem lies and how bad it is, doctors can develop a personalized treatment plan for each patient. That level of precision means the only veins affected can be treated, while the surrounding tissue is left untouched to yield better results.
Real-time guidance during procedures is facilitated by advanced imaging, further boosting safety and accuracy. Now, the integration of diagnostic and treatment technologies can finally take a substantial step forward in vascular medicine.
Endovenous Laser Therapy and Radiofrequency Ablation
Endovenous laser therapy and radiofrequency ablation are among the most common minimally invasive treatments. Both methods utilize thermal energy to seal damaged veins from the inside.
The procedure involves inserting a thin catheter into the affected vein with ultrasound guidance. Laser or radiofrequency energy is then passed through the catheter, heating up the vein walls until they collapse and seal themselves shut. Eventually, the body absorbs the treated vein and reroutes blood through healthier channels.
These are very successful procedures that work better than others for closure of larger varicosities. They also involve only small entry points and minimal anesthesia, which means patients feel less discomfort than is typical after conventional surgery.
Advances in catheter design and energy delivery systems continue to improve the efficiency and precision of these therapies, leading to increased patient outcomes.
Sclerotherapy and Chemical Closure Techniques
Another less invasive option, especially for smaller veins like spider veins, is sclerotherapy. This process entails the injection of a special fluid into the targeted vein, prompting it to collapse and gradually become visible.
Sclerotherapy has also become a more effective treatment due to the recent ability to inject deeper veins with ultrasound guidance. This enables physicians to address veins that are not visible on the skin, thus broadening the scope of conditions manageable without surgery.
Besides classic sclerotherapy, other newer chemical closure techniques use medical adhesives to seal the veins. These techniques do not depend on the application of thermal energy, and they may also decrease the need for post-procedure compression therapy.
The development of these techniques shows how innovation keeps adding to the options for vein treatment.
Enhancing Patient Experience and Recovery
Minimally invasive vein treatment offers a very wide patient experience as one of its most significant benefits. Conventional surgery typically involved general anesthesia, hospital admissions and long recovery times. By comparison, modern procedures generally take place in outpatient settings and allow patients to return home the same day.
Recovery times are shorter, as many patients return to their normal lives in a day or two. Immediate walking is often encouraged post-treatment to help promote normal circulation and encourage the healing process.
Less pain and quicker recovery ultimately lead to increased patient satisfaction and improved compliance with treatment plans. These are key contributors to successful long-term outcomes.
Specialized Venous Clinic Role
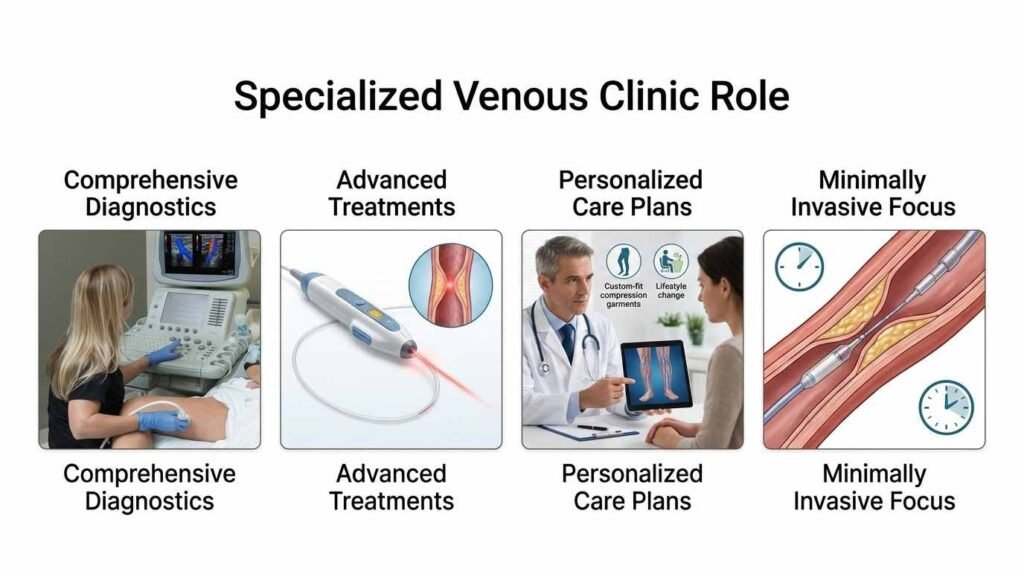
Specialized vein clinics have emerged at the forefront of high-quality vascular care as technology has advanced. In a vein clinic, all of these sophisticated diagnostic tools are put to use by medical professionals who specialize in vein health.
Our patients find experts in care for a variety of treatment options through Texas Vein Experts, and patients benefit from new technology aimed at accurate diagnoses and effective minimally invasive treatments. Specialized centers have the most up-to-date equipment and are likely to follow evidence-based protocols, which collectively lead to patients receiving the best care available.
These clinics provide specialized treatment plans that cater to each patient’s specific needs, all while focusing on vascular conditions.
Reducing Risk of Recurrence and Supporting Recovery
Although minimally invasive treatments are very effective, long-term vein health needs to be maintained. Recurrent disease can be prevented by the treatment of related lifestyle factors, including activity, weight and hydration.
Movement on a regular basis helps to stimulate circulation and support the muscles that aid venous blood flow. Keeping a healthy weight reduces pressure in the veins, while elevating your legs when sitting down will help reduce swelling.
Patients typically follow post-treatment directions of their healthcare providers. These may include the use of compression stockings as needed for a limited time and avoiding long periods of inactivity.
With the right balance of medical care and healthy living, we can safeguard our vascular well-being and minimise the chances of future complications.
Conclusion
This has been a game-changer in the way vascular conditions are treated with minimally invasive vein treatments. Vein Diseases – Treatment without Surgery. With the help of advanced imaging, targeted therapies, and innovative techniques, modern medicine is now capable of treating vein disease effectively without major surgery.
Not only have these technological advances improved clinical outcomes, but they have also enhanced the patient experience. The ability to recover sooner, with less discomfort and tailored arrangements, has transformed treatment into a more achievable option for patients.
The advancements technology offers, alongside the expertise of medical professionals, will eventually revolutionize vein care even further, providing new and improved methods for safer, faster and more effective treatment options for those looking to improve their vascular wellness.
Disclaimer
This article is for informational and educational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the guidance of a qualified healthcare provider regarding any medical condition or treatment options. Do not disregard professional medical advice or delay seeking it based on information provided in this content. Individual results may vary, and all medical decisions should be made in consultation with a licensed medical professional.
References
- Gloviczki, P., Comerota, A. J., Dalsing, M. C., et al. (2011). The care of patients with varicose veins and associated chronic venous diseases: Clinical practice guidelines. Journal of Vascular Surgery, 53(5 Suppl), 2S–48S.
- DOI: 10.1016/j.jvs.2011.01.079
- O’Donnell, T. F., Passman, M. A., Marston, W. A., et al. (2014). Management of venous leg ulcers: Clinical practice guidelines. Journal of Vascular Surgery, 60(2 Suppl), 3S–59S.
- DOI: 10.1016/j.jvs.2014.04.049
- Wittens, C., Davies, A. H., Bækgaard, N., et al. (2015). Editor’s Choice – Management of chronic venous disease. European Journal of Vascular and Endovascular Surgery, 49(6), 678–737.
- DOI: 10.1016/j.ejvs.2015.02.007
- van den Bos, R., Arends, L., Kockaert, M., Neumann, M., & Nijsten, T. (2009). Endovenous therapies of lower extremity varicosities: A meta-analysis. Journal of Vascular Surgery, 49(1), 230–239.
- DOI: 10.1016/j.jvs.2008.06.030
- Jia, X., Mowatt, G., Burr, J. M., Cassar, K., Cook, J., & Fraser, C. (2007). Systematic review of foam sclerotherapy for varicose veins. British Journal of Surgery, 94(8), 925–936.
- DOI: 10.1002/bjs.5891
- Bootun, R., Lane, T. R. A., & Davies, A. H. (2016). The advent of non-thermal, non-tumescent techniques for varicose vein treatment. Phlebology, 31(1 Suppl), 5–14.
- DOI: 10.1177/0268355516632601
- Gibson, K., & Ferris, B. (2017). Cyanoacrylate closure of incompetent great saphenous veins. Journal of Vascular Surgery: Venous and Lymphatic Disorders, 5(5), 658–664.
- DOI: 10.1016/j.jvsv.2017.04.008
- Kachlik, D., Pechacek, V., Musil, V., & Baca, V. (2010). The venous system of the lower limb: Structure and function. Acta Chirurgiae Orthopaedicae et Traumatologiae Cechoslovaca, 77(5), 354–362.
- DOI: 10.55095/ACHOT2010/054