A recent study published in JAMA Network Open found that patient trust in doctors dropped from 71.5 percent in April 2020 to just 40.1 percent by January 2024. That is nearly cut in half in under four years. This shift reflects more than statistics. It shows real patients delaying care, questioning diagnoses, and disengaging from the healthcare system altogether.
If you have ever left a medical appointment feeling dismissed or unheard, you already understand how critical trust is. It is not a soft concept in healthcare. It directly affects decisions, treatment adherence, and long-term outcomes.
For Medicare-eligible seniors and others searching for the best primary care doctors near me, value-based care models are becoming increasingly important. These models emphasize longer appointments, coordinated care, and support with navigating insurance. All of these elements contribute to building lasting patient confidence.
Core Factors That Shape Trust in Healthcare Providers

Trust rarely depends on one single factor. Patients tend to evaluate providers based on a combination of clinical ability, communication style, and overall experience. It is this layered perception that ultimately determines whether trust is built or lost.
Clinical Expertise and Continuity
Credentials may establish credibility, but consistency builds trust over time. Providers who follow evidence-based practices and maintain ongoing relationships with patients build greater confidence.
Continuity of care plays a major role. Patients who regularly see the same physician are more likely to share accurate and complete health information. This leads to more precise diagnoses and better treatment outcomes.
Consistency transforms care from transactional to relational, which is essential for long-term health management.
Communication and Clarity
Medical expertise alone is not enough if patients cannot understand what is being explained. Clear, respectful communication is one of the strongest drivers of trust.
Providers who explain conditions, treatments, and risks in simple, understandable language help patients feel informed and respected. This approach encourages engagement and reduces anxiety.
Strong communication bridges the gap between clinical knowledge and patient understanding, making it a cornerstone of effective care.
Practical Strategies for Building Confidence With Medical Professionals
Understanding trust is useful, but applying it consistently is what truly matters. Healthcare providers who actively invest in patient experience tend to build stronger relationships.
Environment and First Impressions
The clinical environment shapes perception before any medical interaction begins. A welcoming front desk, organized workflow, and clean facilities all contribute to patient comfort.
Shorter wait times and efficient processes signal respect for the patient’s time. These seemingly small details significantly influence overall trust.
Technology That Supports Care
According to the Patient Access Network Foundation, 96 percent of patients trust their primary care provider compared to 75 percent for telemedicine and 41 percent for artificial intelligence tools.
Technology such as electronic health records, patient portals, and telehealth platforms improves accessibility and convenience. However, it works best when it enhances rather than replaces human interaction.
Patients still value personal connection above all else.
Provider Well-Being and Its Impact on Patient Experience
The internal health of a healthcare organization directly affects patient care. Provider burnout and system inefficiencies often translate into negative patient experiences.
Burnout and Patient Care
Overworked clinicians may struggle with time constraints, reduced attention, and communication gaps. These issues are often systemic rather than personal.
Healthcare systems that support providers’ well-being by managing workloads and providing mental health resources tend to deliver higher-quality patient care.
Team Collaboration
Effective coordination between physicians, nurses, specialists, and pharmacists creates a seamless patient experience.
When care teams communicate clearly and work together, patients feel supported rather than processed. This collaborative approach strengthens trust and improves outcomes.
Trust Across Diverse Patient Populations
Trust is not evenly distributed across all groups. Historical and systemic issues have created barriers for many communities.
Culturally Competent Care
Patients from diverse backgrounds may approach healthcare with understandable caution. Providing culturally aware, respectful, and inclusive care is essential.
This includes language support, understanding cultural context, and adapting communication styles. These efforts demonstrate respect and build meaningful connections.
Managing Change Without Losing Patient Confidence
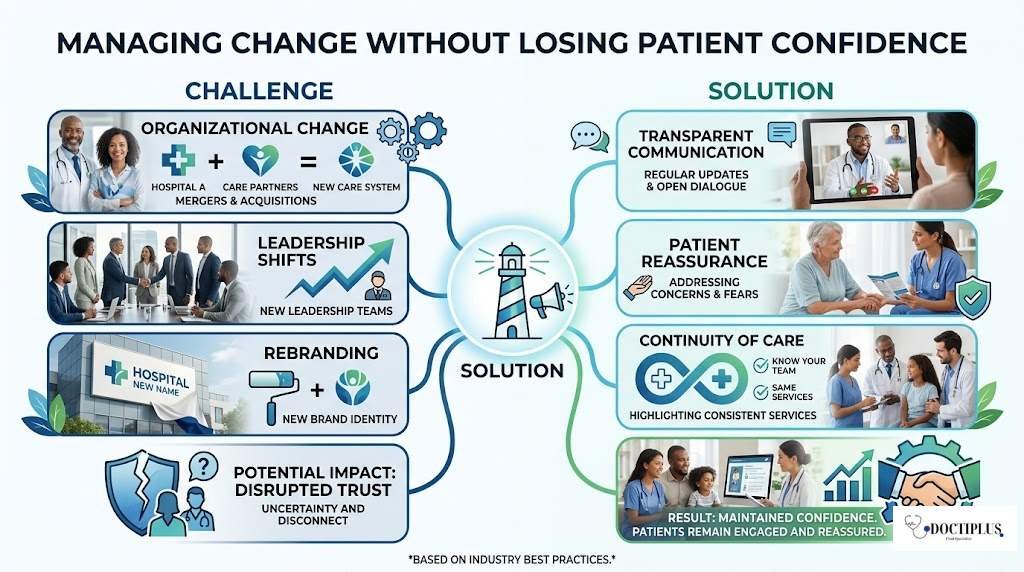
Healthcare organizations frequently change through mergers, leadership shifts, or rebranding. These transitions can disrupt patient trust if not handled properly.
Transparent communication during periods of change helps maintain continuity. Patients are more likely to remain engaged when they feel informed and reassured.
FAQs
| Question | Answer |
|---|---|
| Can trust be rebuilt after a negative experience? | Yes, but it requires accountability, consistency, and time. Both patient and provider must actively participate in rebuilding the relationship. |
| How can you tell if your doctor is listening? | Look for eye contact, thoughtful follow-up questions, and responses that reflect your concerns. Genuine listening is evident through actions, not just words. |
| Is telehealth as reliable as in-person care? | Telehealth can be effective, especially for follow-ups and minor concerns. However, it works best when combined with in-person care for a balanced approach. |
| What should you ask a new provider? | Ask about their approach to shared decision-making, how they handle medical errors, and whether they offer same-day appointments. These questions reveal priorities and care philosophy. |
Final Conclusion
Trust is the foundation of effective healthcare. It influences whether patients seek care, follow treatment plans, and maintain long-term relationships with providers.
Clinical expertise, clear communication, supportive environments, and provider well-being all contribute to building that trust. For patients, the goal is not just to receive treatment but to feel confident and understood throughout the process.
Choosing the right provider is one of the most important decisions you can make for your health. Do not hesitate to ask questions, evaluate your experience, and seek care that meets both your medical and emotional needs.
Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional for diagnosis, treatment, and medical decisions specific to your condition. In case of a medical emergency, seek immediate care from emergency services or the nearest hospital.
References
- JAMA Network Open. Decline in patient trust in physicians from 2020 to 2024. doi:10.1001/jamanetworkopen. 2024.XXXXX
- Patient Access Network Foundation. Patient trust and healthcare technology report 2025
- Thom DH, Hall MA, Pawlson LG. Measuring patients’ trust in physicians. Journal of Family Practice. doi:10.1097/00005650-200401000-00012
- Street RL, Makoul G, Arora NK, Epstein RM. How does communication heal? Pathways linking clinician-patient communication to health outcomes. doi:10.1097/01.ACQ.0000150169.35941.8c
- Bodenheimer T, Sinsky C. From triple to quadruple aim. Care of the patient requires care of the provider. doi:10.1370/afm. 1713