According to the American Dental Association’s 2024 consumer survey, nearly 37 million Americans used a teeth whitening product in the past year, yet roughly one in four experienced gum irritation during the process. As professional whitening treatments become more accessible and at-home products grow increasingly potent, the challenge of achieving a brighter smile while protecting already sensitive gum tissue has become a real concern for millions of people.
The stakes matter more than many realize. Gum sensitivity is not just about temporary discomfort. It can signal underlying inflammation that whitening agents might exacerbate, potentially leading to more serious periodontal issues down the line. For individuals who already experience gum tenderness during routine brushing or flossing, the decision to whiten requires careful consideration of both immediate safety and long-term oral health.
Understanding how whitening agents interact with gum tissue, which products minimize risk, and what protective measures actually work can mean the difference between achieving your cosmetic goals safely and dealing with weeks of painful inflammation. The key lies in recognizing that not all whitening approaches are created equal, and that the right strategy depends on understanding the specific mechanisms at play.
How Teeth Whitening Affects Gum Health and Causes Sensitivity
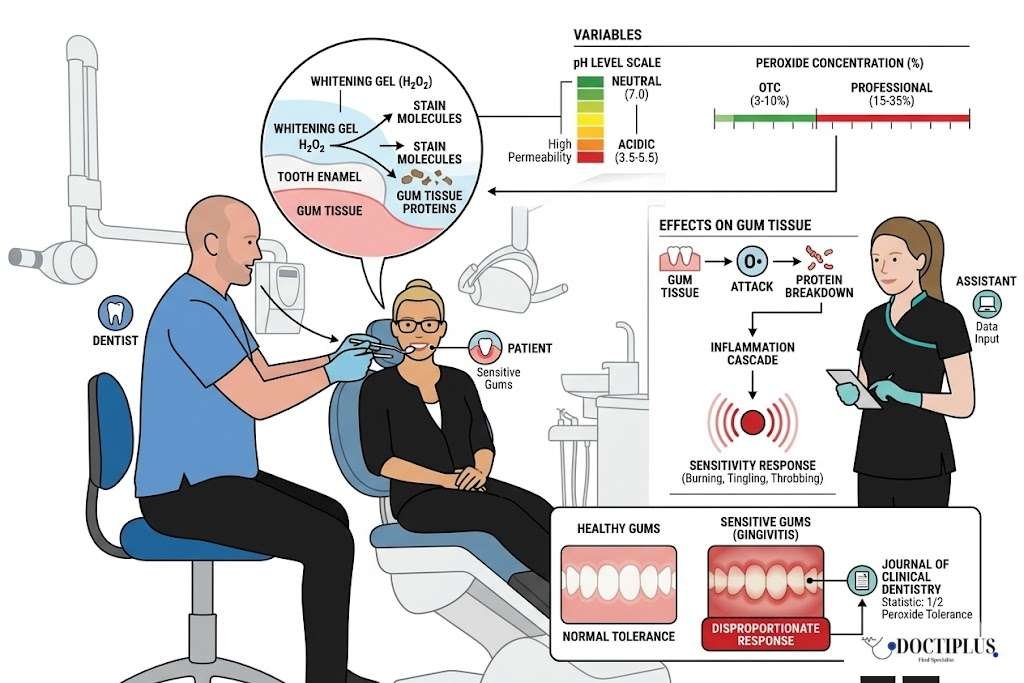
The chemistry behind teeth whitening creates a predictable cascade of reactions that directly impact gum tissue, particularly in individuals who already experience sensitivity. Most whitening products rely on hydrogen peroxideor carbamide peroxide as their active ingredients. These compounds break down into oxygen radicals that penetrate tooth enamel and break apart stain molecules.
Why Peroxide Irritates Gum Tissue
Here is where the gum sensitivity enters the picture: these same oxygen radicals do not distinguish between stained tooth surfaces and the delicate epithelial cells that line your gums. When whitening gel comes into contact with gum tissue, whether through poorly fitted trays, gel overflow, or direct application via strips, the peroxide begins breaking down proteins in the gum’s surface layer. This process triggers an inflammatory response that manifests as the burning, tingling, or throbbing sensation many people experience.
Role of Concentration and Exposure Time
The concentration factor amplifies everything. Professional treatments typically use 15 to 35 percent hydrogen peroxide, while over-the-counter products range from 3 to 10 percent. But even lower concentrations can cause significant gum irritation in sensitive individuals, especially when exposure time exceeds the tissue’s tolerance. Consider someone using whitening strips designed to stay on for 30 minutes. If those strips extend slightly beyond the tooth surface onto the gum line, that is 30 minutes of continuous chemical contact with tissue that is already prone to inflammation.
How pH Levels Affect Gum Permeability
The pH level of whitening formulations plays an equally critical role. Many whitening products have an acidic pH (3.5-5.5), which temporarily softens tooth enamel, allowing better peroxide penetration. Unfortunately, this acidic environment also increases gum tissue permeability, allowing the peroxide to penetrate deeper into the gingival tissues and potentially reach nerve endings that trigger pain responses.
What makes this particularly challenging for people with pre-existing gum sensitivity is that their tissue is already in a heightened state of reactivity. The inflammatory pathways are essentially primed, meaning even minimal exposure to whitening agents can trigger disproportionate responses. Research published in the Journal of Clinical Dentistry shows that individuals with existing gingivitis experience gum irritation at roughly half the peroxide concentration required to affect healthy gum tissue.
Understanding these mechanisms reveals why blanket advice about safe whitening often falls short. The interaction between whitening chemistry and individual gum health creates a highly personalized equation that requires more nuanced approaches than one-size-fits-all products typically provide.
Comparing Teeth Whitening Methods for Sensitive Gums
Professional Whitening Treatments Versus Over-the-Counter Products
Professional whitening treatments offer several distinct advantages for individuals with sensitive gums, starting with customized application techniques that minimize gum exposure. Dental professionals use precisely fitted trays created from impressions of your teeth, ensuring the whitening gel stays exactly where it belongs rather than seeping onto gum tissue. Additionally, professional treatments often include protective barriers, thin resin dams or specialized gels, applied directly to the gum line before whitening begins.
The concentration control factor works differently than most people assume. While professional treatments use higher peroxide concentrations (15 to 35 percent versus 3 to 10 percent in store products), the controlled application and shorter exposure times often result in less overall gum irritation. A typical in-office session lasts 15 to 20 minutes under professional supervision, compared to the 30 to 60-minute exposure times common with at-home strips or trays that may not fit properly.
Over-the-counter products present a more complex risk profile for sensitive gums. Whitening strips, while convenient, pose the highest risk of gum contact because they are manufactured in standard sizes that rarely match individual tooth dimensions. The adhesive backing can also cause mechanical irritation along the gum line. Custom-fitted trays purchased from dental offices but used at home with lower-concentration gels represent a middle-ground option, offering better fit than strips while allowing gradual whitening that sensitive individuals often tolerate better.
Natural and Alternative Whitening Options for Sensitive Gums
Natural whitening approaches appeal to many people with sensitive gums, though their effectiveness varies significantly. Oil pulling with coconut oil has gained attention for its dual benefits: mild whitening from plaque removal and anti-inflammatory properties that may soothe sensitive gums. While the whitening effect is subtle compared to peroxide-based products, the process does not introduce chemical irritants.
Whitening toothpastes formulated specifically for sensitive teeth often contain potassium nitrate or stannous fluoride, along with mild abrasives. These ingredients can help desensitize both tooth and gum tissue over time, though the whitening results typically require several months of consistent use. The trade-off is minimal risk of acute gum irritation.
Professional teeth whitening in Fort Lauderdale: practitioners increasingly offer alternative approaches, such as light-activated systems with lower peroxide concentrations or gradual whitening protocols that spread treatment over multiple sessions. These methods allow practitioners to monitor gum response and adjust accordingly, making them particularly suitable for patients with documented gum sensitivity issues.
Hydrogen peroxide alternatives, such as sodium bicarbonate-based systems or PAP (phthalimidoperoxycaproic acid) formulations, are emerging as gentler options. PAP-based whiteners work through a different chemical pathway that does not rely on the aggressive oxidation process of traditional peroxides, potentially reducing gum irritation while still achieving measurable whitening results.
Quick Comparison of Whitening Options
- In-office professional whitening: highest peroxide concentration, shortest exposure, best gum protection with barriers.
- Dentist-supplied custom trays at home: moderate concentration, good fit, lower irritation risk than strips.
- Whitening strips: convenient but poor fit increases gum contact and mechanical irritation.
- Whitening toothpaste with potassium nitrate: slowest results, lowest risk of gum irritation.
- PAP-based whiteners: gentler chemistry, suitable for those who cannot tolerate peroxide.
- Oil pulling and natural methods: subtle whitening, minimal risk, often soothing for inflamed gums.
Preventive Measures to Protect Sensitive Gums During Whitening

Using Custom-Fitted Trays and Safer Formulations
The single most effective strategy for protecting sensitive gums during whitening involves precision application through properly fitted trays that create clear boundaries between whitening agents and gum tissue. Custom trays fabricated by dental professionals feature reservoirs that hold gel away from the gum line while maintaining contact with tooth surfaces. This design prevents gel overflow, which is the main cause of whitening-related gum irritation.
When selecting whitening formulations, concentration matters less than pH balance for gum-sensitive individuals. Products with neutral pH (around 7.0) or those containing buffering agents cause significantly less gum irritation than highly acidic formulations, even when the peroxide concentration is identical. Some professional-grade formulations include desensitizing agents, such as potassium nitrate, mixed directly into the whitening gel, providing protection during the whitening process rather than requiring a separate treatment.
The timing strategy also requires adjustment for sensitive gums. Rather than following standard application times, individuals with gum sensitivity often achieve better results with shorter, more frequent sessions. A 10 to 15-minute application every other day typically causes less cumulative irritation than 30-minute sessions performed consecutively, while still allowing the whitening chemistry to work effectively over time.
Pre-Whitening Gum Care and Oral Hygiene Adjustments
Preparing sensitive gums for whitening treatment begins 1 to 2 weeks before the first application through targeted anti-inflammatory protocols. Using toothpaste containing stannous fluoride or switching to an antimicrobial mouth rinse helps reduce baseline gum inflammation, creating a more stable foundation for whitening treatment.
Oral hygiene modifications during the pre-whitening phase can significantly impact treatment tolerance. Switching to an extra-soft toothbrush and incorporating gentle gum massage with vitamin E oil or aloe vera gel helps improve gum tissue resilience. Some dental professionals recommend a brief course of professional-grade fluoride gel applied with custom trays to strengthen both tooth structure and adjacent gum tissue.
The dietary preparation aspect is often overlooked but is crucial for gum-sensitive individuals. Avoiding acidic foods and beverages for 48 hours before whitening helps maintain optimal tissue pH. Additionally, staying well-hydrated and ensuring adequate vitamin C intake support the repair mechanisms of gum tissue that may be needed during the whitening process.
Preventive Checklist Before Starting Whitening
- Schedule a dental exam to rule out active gingivitis or periodontitis.
- • Switch to a desensitizing toothpaste with potassium nitrate 2 weeks in advance.
- Use a soft-bristled toothbrush and avoid aggressive brushing.
- Avoid acidic drinks such as citrus juice, soda, and wine for 48 hours before treatment.
- Request custom trays rather than stock trays or strips when possible.
- Choose a pH-neutral or buffered whitening gel.
- Start with a lower concentration and shorter session length.
Scientific Evidence on Whitening and Gum Sensitivity
Clinical research on whitening-induced gum sensitivity has evolved significantly over the past decade, providing clearer guidance on safe practices for vulnerable individuals. A 2023 study published in the Journal of Clinical Periodontology followed 180 participants with pre-existing gum sensitivity through various whitening protocols, finding that the application method influenced gum irritation more than the concentration level. Participants using properly fitted trays experienced gum irritation in only 12 percent of cases, compared to 47 percent among those using over-the-counter strips.
Importance of pH in Whitening Product Safety
The pH factor has emerged as particularly significant in recent research. Studies conducted at the University of Michigan’s dental school demonstrated that whitening gels with a pH above 6.5 caused 60% less gum irritation than acidic formulations (pH 3.5 to 4.5), even when using identical peroxide concentrations. This finding has prompted several manufacturers to reformulate their products with buffering agents that maintain higher pH levels throughout the whitening process.
Long-Term Safety of Repeated Whitening Treatments
Long-term studies on the cumulative effects of gum have yielded reassuring results for most individuals. Research tracking patients over five years of periodic whitening treatments found no permanent gum damage in participants who experienced temporary sensitivity during treatment. However, the data revealed an important distinction: individuals who continued whitening despite ongoing gum pain showed measurably more gum recession than those who paused treatment until sensitivity resolved.
Ingredients That Increase the Risk of Gum Irritation
Ingredient-specific research has identified particular compounds that correlate with higher gum sensitivity rates. Products containing citric acid as a penetration enhancer showed 40% higher rates of gum irritation than formulations using alternative penetration methods. Similarly, whitening products with alcohol-based carriers showed greater gum sensitivity than glycerin-based alternatives, prompting formulation changes across several major brands.
How Treatment Frequency Impacts Gum Recovery
The frequency factor has received considerable attention in recent clinical trials. A study published in the International Journal of Dental Hygiene compared daily versus every-other-day whitening protocols in individuals with gum sensitivity. The alternate-day approach yielded equivalent whitening outcomes with 35% less gum irritation, suggesting that the time between applications may be as important as the whitening chemistry itself.
Emerging studies on biomarker analysis are beginning to identify individuals at the highest risk for whitening-induced gum sensitivity before treatment begins. Saliva testing for specific inflammatory markers may eventually allow practitioners to predict gum sensitivity and adjust whitening protocols accordingly, though these tests remain in research phases.
Managing Gum Sensitivity After Whitening Treatment
When gum sensitivity does occur despite preventive measures, the immediate response strategy significantly influences both comfort and recovery time. The most effective first step is thorough rinsing with lukewarm water to remove any residual whitening agent, followed by gentle application of an anti-inflammatory gel containing ingredients such as aloe vera or chamomile extract.
Professional Treatments That Speed Up Recovery
Professional-grade desensitizing treatments offer faster relief than over-the-counter alternatives. Fluoride varnishes applied by dental professionals create a protective barrier over irritated gum tissue while delivering sustained anti-inflammatory benefits. Some practitioners use low-level laser therapy to accelerate the healing of gum tissue. Studies suggest this approach can reduce recovery time from 5 to 7 days down to 2 to 3 days for most individuals.
Home Aftercare Routine for Irritated Gums
The aftercare routine requires specific modifications during the recovery period. Switching to an alcohol-free antimicrobial rinse prevents additional tissue irritation while maintaining oral hygiene. Cold compresses applied externally for 10 to 15 minute intervals can provide significant pain relief, though ice should never be applied directly to gum tissue.
Foods to Eat and Avoid During Gum Recovery
Dietary adjustments during recovery prove particularly important for preventing secondary irritation. Avoiding hot beverages, spicy foods, and acidic fruits allows irritated tissue to heal without additional chemical stress. Many people find that cold, soft foods like yogurt or smoothies provide comfort while supporting the healing process.
- Recommended: yogurt, smoothies, mashed potatoes, oatmeal, cold soups, bananas.
- Avoid: citrus fruits, tomato sauce, hot coffee, chili, vinegar dressings, carbonated drinks.
When to Modify or Stop Your Whitening Protocol
For individuals who experience repeated gum sensitivity with whitening treatments, the solution often lies in modifying the protocol rather than abandoning whitening altogether. Working with dental professionals to develop personalized whitening schedules, perhaps alternating whitening weeks with recovery periods, allows many gum-sensitive individuals to achieve their cosmetic goals safely over extended timeframes.
Final Conclusion
Teeth whitening can be safe for people with sensitive gums, but only when the approach is tailored to individual tissue tolerance rather than following generic instructions on a product box. The evidence is clear on three points. First, application method matters more than peroxide concentration, so custom-fitted trays and professional barriers dramatically reduce gum irritation. Second, pH balance and ingredient choice can be the deciding factor between comfortable treatment and painful inflammation. Third, recovery time between sessions is not optional for sensitive individuals; it is part of the protocol.
If your gums already react to normal brushing, skip the aggressive over-the-counter strips and start with a dentist-led plan. A short consultation can identify whether underlying gingivitis needs to be treated first, which whitening chemistry suits your tissue, and how to schedule sessions so your gums heal between applications. Patience, the right formulation, and a properly fitted tray will almost always produce a brighter smile without the burning, tingling, and recession that poorly chosen products cause. A whiter smile is worth achieving, but never at the cost of long-term gum health.
Medical Disclaimer
The information provided in this article is for general educational and informational purposes only. It is not intended as a substitute for professional medical, dental, or periodontal advice, diagnosis, or treatment. Always seek the advice of your dentist, periodontist, or other qualified healthcare provider with any questions you may have regarding teeth whitening, gum sensitivity, or any medical condition. Never disregard professional advice or delay seeking it because of something you have read here. Individual results from whitening treatments vary, and products or procedures suitable for one person may not be appropriate for another. Reliance on any information provided in this article is solely at your own risk.
References
- American Dental Association. (2024). Consumer Survey on Oral Health and Cosmetic Dentistry. ADA Health Policy Institute.
- Journal of Clinical Periodontology. (2023). Application Method and Gingival Response in Patients with Pre-Existing Sensitivity: A 180-Participant Trial.
- University of Michigan School of Dentistry. (2022). pH Balance and Gingival Irritation in Peroxide-Based Whitening Gels.
- International Journal of Dental Hygiene. (2023). Comparative Outcomes of Daily Versus Alternate-Day Whitening Protocols in Sensitive Patients.
- Journal of Clinical Dentistry. (2022). Inflammatory Thresholds in Gingivitis Patients Exposed to Hydrogen Peroxide Whitening Agents.
- American Academy of Periodontology. (2024). Clinical Guidelines on Cosmetic Procedures for Patients with Periodontal Sensitivity.
- Journal of Esthetic and Restorative Dentistry. (2023). Phthalimidoperoxycaproic Acid (PAP) as an Alternative to Hydrogen Peroxide in Tooth Whitening.
- British Dental Journal. (2022). Long-Term Gingival Outcomes After Five Years of Periodic Whitening Treatment.