Benzodiazepines are among the most widely prescribed medications in the United States. Drugs like Xanax, Klonopin, Valium, and Ativan are used to treat anxiety, panic disorders, seizures, and insomnia. They work by slowing activity in the central nervous system, producing a calming effect that many people find relief in.
In this article, Doctiplus explores what happens when someone takes a benzodiazepine alongside a recreational drug. In short: nothing good. Depending on the combination, the risks range from uncomfortable to life-threatening. And because benzodiazepines are so common, these combinations happen more often than most people realize.
Why Benzodiazepines Are Particularly Dangerous to Mix
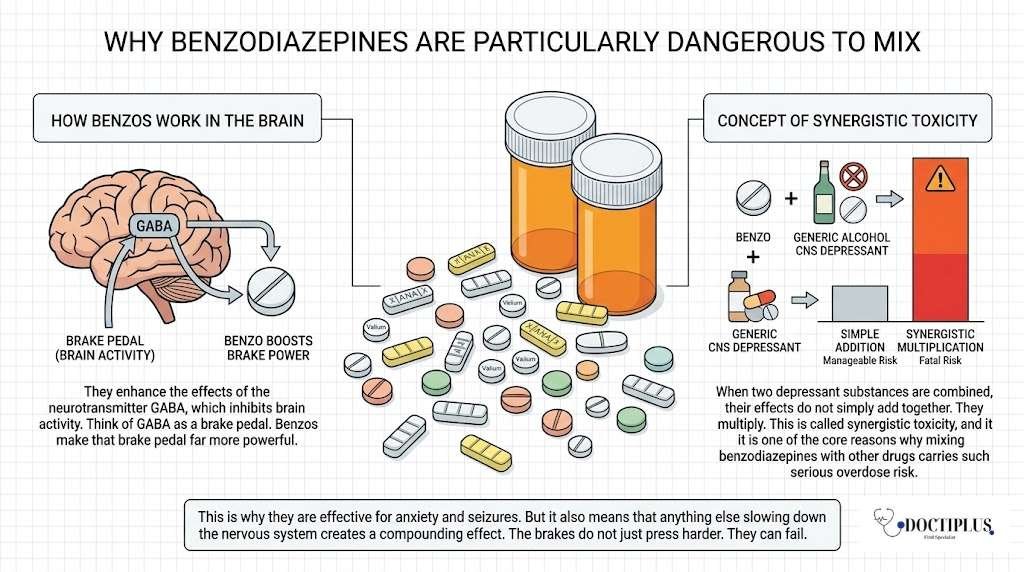
How Benzos Work in the Brain
To understand the danger, it helps to know what benzodiazepines are actually doing inside the body. They enhance the effects of the neurotransmitter GABA, which inhibits brain activity. Think of GABA as a brake pedal. Benzos make that brake pedal far more powerful.
This is why they are effective for anxiety and seizures. But it also means that anything else slowing down the nervous system creates a compounding effect. The brakes do not just press harder. They can fail.
Concept of Synergistic Toxicity
When two depressant substances are combined, their effects do not simply add together. They multiply. This is called synergistic toxicity, and it is one of the core reasons why mixing benzodiazepines with other drugs carries such serious overdose risk. A dose of each substance that would be manageable on its own can become fatal in combination.
Mixing Benzodiazepines With Alcohol
Alcohol is the most common substance mixed with benzodiazepines, and one of the most dangerous. Both are central nervous system depressants. When taken together, they dramatically increase the risk of respiratory depression, the slowing of breathing that is the primary cause of overdose death.
What Respiratory Depression Actually Looks Like
A person experiencing respiratory depression from a benzodiazepine-alcohol combination may become extremely drowsy, confused, and unresponsive. Breathing slows to the point where the body does not receive enough oxygen. This can lead to brain damage, cardiac arrest, or death. The person may not appear distressed. They may fall asleep and not wake up.
Even moderate drinking while taking a prescribed benzodiazepine raises this risk. This combination is not reserved for people taking large doses.
Opioids and Benzodiazepines: A Well-Documented Deadly Pair
Why This Combination Drives Overdose Statistics
The combination of opioids and benzodiazepines has been called one of the most dangerous drug interactions in modern medicine. Both classes of drugs slow breathing, and together they are responsible for a substantial portion of overdose deaths in the United States. The FDA has issued its strongest warning label, a black box warning, specifically about this combination.
Opioids and benzodiazepines are frequently co-prescribed, which makes this particularly complex. A person managing chronic pain with opioids who is also prescribed a benzo for anxiety may not fully understand the elevated risk they are carrying. This is why transparent communication with prescribing physicians matters so much.
Stimulants and Benzos: False Safety and Cardiac Strain
What Happens When You Mix Uppers and Downers
Some people mistakenly believe that combining a stimulant with a depressant balances things out. It does not. When stimulants like cocaine or amphetamines are combined with benzodiazepines, the drugs do not cancel each other out. Instead, the heart and cardiovascular system simultaneously absorb competing signals. This creates significant strain, irregular heart rhythms, and unpredictable neurological effects.
One particularly concerning pattern seen in emergency settings involves combining meth and benzodiazepines. In this combination, methamphetamine aggressively elevates heart rate and blood pressure while the benzodiazepine masks the warning signs a person would normally feel, such as chest pain, racing heart, or dizziness. The result is that someone can be in serious cardiac distress without knowing it until the situation becomes an emergency.
MDMA, Psychedelics, and Benzos
A More Complex Interaction
People sometimes take benzodiazepines to reduce anxiety or “come down” after using MDMA or psychedelics like psilocybin or LSD. While the risk profile is different from opioid combinations, this practice is not without concern.
Benzodiazepines blunt the psychological experience of these substances, which may seem appealing in a difficult moment. But they also impair judgment and memory formation, and using them to manage a bad trip can delay someone from seeking actual help. There is also limited research on how benzodiazepines interact with MDMA’s cardiovascular effects, which already include elevated heart rate and temperature.
Cannabis and Benzodiazepines
What People Often Underestimate
Cannabis is frequently perceived as low-risk, and in many contexts it is. But mixing marijuana with Xanax is something that deserves more caution than it typically receives. Both substances can cause sedation, cognitive impairment, and decreased coordination. Combined, they amplify each other’s sedating effects and can significantly impair a person’s ability to drive or respond to emergencies.
There is also evidence that cannabis can affect how the liver processes certain benzodiazepines, potentially increasing blood levels and extending the drug’s effects beyond what was expected.
Who Is Most at Risk
Factors That Elevate Danger
Certain populations face heightened risk when benzodiazepines and recreational drugs are combined. Older adults metabolize medications more slowly, meaning substances stay in the system longer and at higher effective concentrations. People with underlying cardiac or respiratory conditions face compounded physical risk. Those with a history of substance use disorder may be using higher doses of recreational drugs than someone without that history.
People who obtain benzodiazepines outside of medical supervision also face a distinct danger: they may not know what they are actually taking. Counterfeit pills containing fentanyl or other synthetic opioids have been found in illicitly distributed pills that look like common benzos. This is a relatively recent but devastating development in the overdose crisis.
Recognizing an Overdose and Getting Help
Signs That Require Immediate Action
If someone has combined a benzodiazepine with another substance and shows any of the following signs, call 911 immediately: unresponsive to voice or touch, very slow or stopped breathing, blue or gray lips or fingertips, pinpoint pupils, or a limp body. Time matters. Do not wait to see if the person improves on their own.
Naloxone, commonly known as Narcan, can reverse opioid overdose but does not reverse benzodiazepine overdose. However, if there is any chance opioids are involved, administering naloxone is still the right call and can buy time until emergency responders arrive.
Having Honest Conversations About Prescription Use
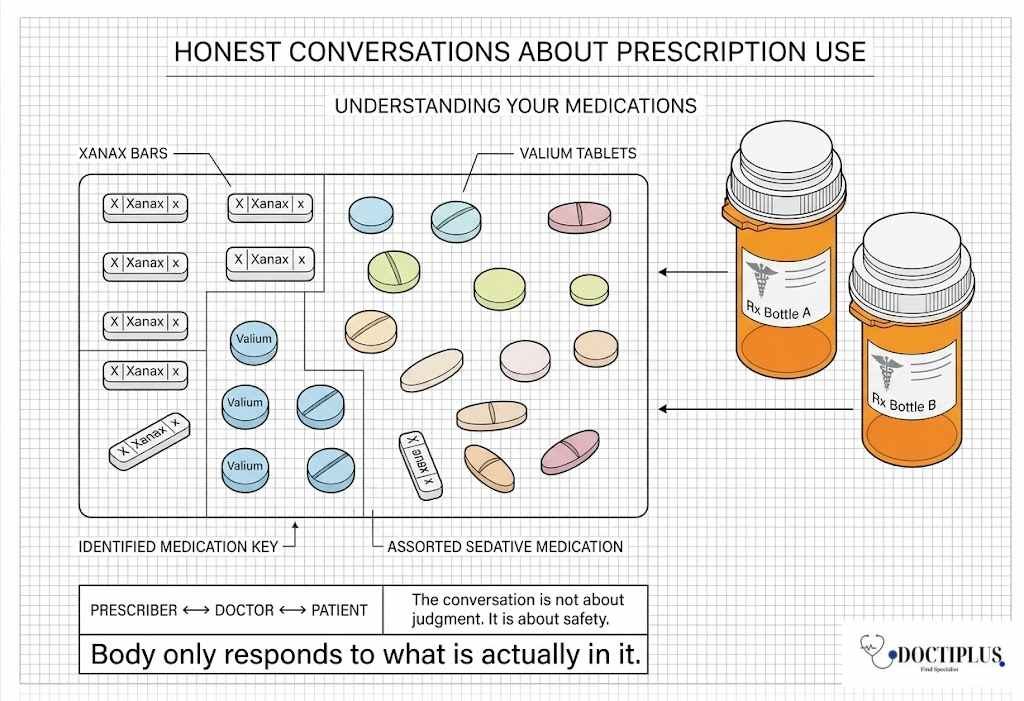
If you are prescribed a benzodiazepine and you use recreational substances, it is worth having an honest conversation with your prescriber. That conversation is not about judgment. It is about safety.
Your doctor cannot make informed decisions about your care without accurate information. There are often alternatives, adjusted dosing strategies, or harm reduction approaches that can reduce your risk while still addressing the conditions you are being treated for.
Benzodiazepines are legitimate and often effective medications. The risks discussed here are not reasons to fear them in an appropriate clinical setting. There are reasons to take the interactions seriously, because the body does not distinguish between what was prescribed and what was recreational. It only responds to what is actually in it.
Final Conclusion
Benzodiazepines can be highly effective medications when used correctly under medical supervision, but they become far more dangerous when mixed with recreational substances. Whether combined with alcohol, opioids, stimulants, cannabis, or party drugs, the results are often unpredictable and can quickly escalate into medical emergencies. Many people underestimate these risks because the substances involved may be common, legal, or familiar.
The safest approach is awareness, honesty, and caution. If you are prescribed a benzodiazepine, always understand how it interacts with anything else you may take. If recreational substances are part of your life, discussing that openly with a healthcare provider can significantly reduce harm. When it comes to benzodiazepines, dangerous outcomes often happen not because people intended harm, but because they underestimated the combination.
Disclaimer
This article is for educational and informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional regarding medications, substance use, or health concerns. If you suspect an overdose or medical emergency, call your local emergency services immediately.
References
- U.S. Food and Drug Administration (FDA). Boxed Warning for Opioids and Benzodiazepines Combined Use.
- National Institute on Drug Abuse (NIDA). Benzodiazepines and Opioids.
- Centers for Disease Control and Prevention (CDC). Risks of Combining Sedatives and Opioids.
- Substance Abuse and Mental Health Services Administration (SAMHSA). Overdose Prevention and Naloxone Guidance.
- National Library of Medicine. Benzodiazepine Toxicity and Drug Interactions.
- Doctiplus Editorial Research Team. Clinical review and educational summary on benzodiazepine interaction risks.