According to the American Association of Oral and Maxillofacial Surgeons, roughly 85 percent of wisdom teeth require removal at some point. Yet, the days following extraction often catch patients off guard with unexpected swelling that can affect everything from their ability to speak clearly to their confidence returning to work or school. As dental practices increasingly emphasize personalized recovery protocols and patients seek faster return to normal activities, understanding how to manage post-surgical swelling has become crucial for optimal healing outcomes.
The challenge extends beyond simple discomfort. Excessive or poorly managed swelling can delay tissue healing, increase the risk of infection, and prolong the overall recovery timeline. For anyone facing wisdom tooth extraction, whether it is a straightforward removal or a complex impacted tooth situation, knowing the specific steps that minimize swelling can mean the difference between a smooth three-day recovery and weeks of ongoing complications.
What follows is not generic post-op advice, but targeted strategies based on how swelling actually develops after oral surgery and which interventions research shows work best during each phase of healing.
How Does Swelling Occur After Wisdom Teeth Removal?
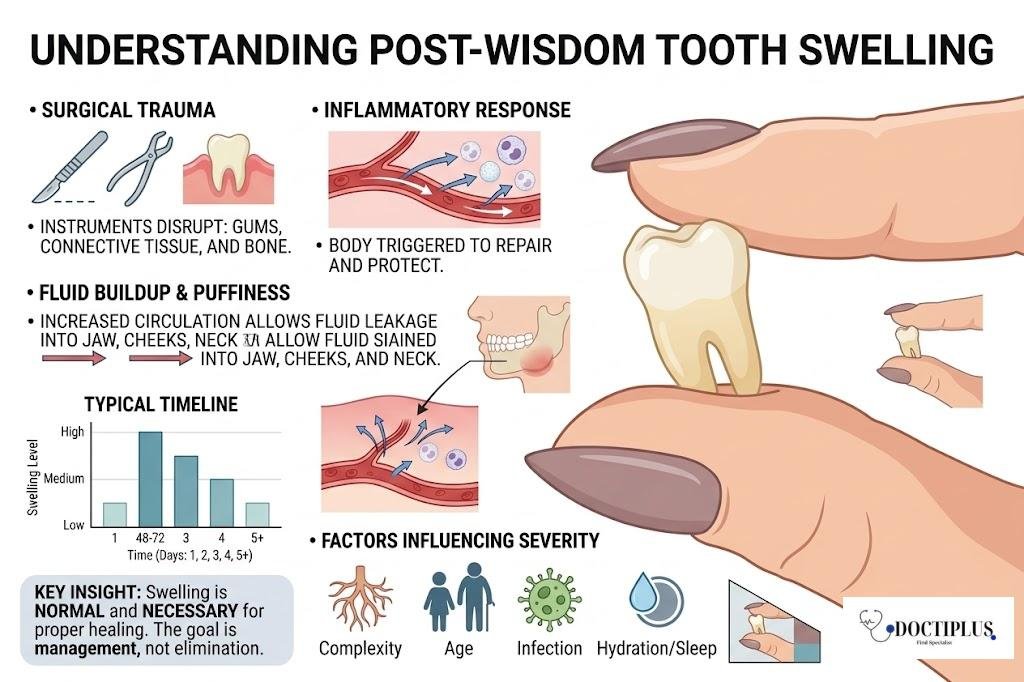
Understanding why swelling happens helps explain why certain management techniques work better than others. During wisdom tooth extraction, surgical instruments necessarily disrupt surrounding tissues, including gums, connective tissue, and, sometimes, bone. Your body interprets this disruption as an injury and immediately triggers an inflammatory response to protect the area and initiate healing.
Inflammatory Response and Fluid Buildup
This inflammatory cascade involves increased blood flow to the extraction site, which brings infection-fighting white blood cells and healing nutrients to the area. However, the increased circulation also allows fluid to leak from blood vessels into surrounding tissues, creating the characteristic puffiness around your jaw, cheeks, and sometimes extending toward your neck.
Typical Swelling Timeline After Extraction
The timeline follows a predictable pattern. Swelling typically peaks 48 to 72 hours after surgery, then gradually subsides over the following week. Lower wisdom teeth generally cause more swelling than upper ones because the tissue density differs, and gravity affects fluid accumulation. Impacted teeth requiring bone removal create more tissue trauma and correspondingly more swelling than simple extractions.
Factors That Influence Swelling Severity
Several factors influence severity beyond the complexity of your specific procedure. Age plays a role, as younger patients often experience less swelling and faster resolution. Pre-existing inflammation from infected or problematic wisdom teeth can intensify the post-surgical response. Even your hydration status and sleep quality in the days leading up to surgery affect how your body manages the inflammatory response.
The key insight here is that some degree of swelling is both normal and necessary for proper healing. The goal is not to eliminate it, but to keep it within manageable bounds while supporting your body’s natural repair mechanisms.
What Are the Best Tips to Reduce Swelling After Surgery?
Effective swelling management starts immediately after your procedure and involves a combination of temperature therapy, positioning, activity modification, and strategic nutrition support. The most impactful interventions work by either reducing the inflammatory response directly or helping your body process accumulated fluids more efficiently.
Why Temperature Therapy Matters Most Early On
Temperature management forms the foundation of early swelling control. Cold therapy constricts blood vessels, limiting the fluid accumulation that creates visible swelling. However, the application method and timing matter significantly. Many patients make the mistake of applying ice directly to the skin or using it inconsistently, which reduces effectiveness and can even cause tissue damage.
Positioning and Rest for Faster Recovery
Beyond cold therapy, elevation and rest work together to leverage gravity in your favor. When you lie flat or keep your head at the same level as your heart, fluid pools in the extraction area. Simple positioning changes can dramatically impact how much swelling develops during those critical first 72 hours.
Activity level during early recovery also influences outcomes more than most patients realize. While complete bed rest is not necessary, understanding which movements and activities increase blood flow to your head helps you make better choices about returning to normal routines.
How Do Ice Packs and Rest Help Limit Swelling?
Correct Ice Pack Technique After Oral Surgery
Proper ice application involves 20 minutes on, 20 minutes off cycles during the first 48 hours after surgery. Use a thin cloth barrier between the ice pack and your skin to prevent cold injury, and focus the cold therapy on the external area over the extraction site rather than cooling your entire face. Commercial gel packs that remain flexible when frozen often work better than rigid ice packs because they conform to your facial contours.
The 20-minute cycle timing is not arbitrary. It takes about that long for cold therapy to penetrate tissue and begin affecting blood vessel diameter. Longer applications do not increase benefits but can damage skin. After 48 hours, switch to warm compresses to increase circulation and encourage the body to process accumulated fluids.
Head Elevation During Sleep and Rest
Head elevation during sleep and rest periods significantly impacts overnight swelling development. Prop yourself up with multiple pillows so your head remains above heart level. Even a 30-degree angle makes a meaningful difference. Many patients find sleeping in a recliner for the first few nights more comfortable and effective than trying to maintain elevation in bed.
Activities to Avoid in the First 72 Hours
Rest during the first 72 hours means avoiding activities that raise blood pressure or require repeated bending. Skip intense exercise, heavy lifting, or prolonged periods with your head down. These activities increase blood flow to your head and can worsen swelling or trigger bleeding.
- Avoid running, gym workouts, and strenuous cardio.
- Skip heavy lifting, yard work, and moving furniture.
- Do not bend over repeatedly to pick up items from the floor.
- Pause yoga poses that place the head below the heart.
- Limit long phone calls or talking that strains the jaw.
Why Is Hydration Important During Recovery?
Adequate hydration helps your lymphatic system process the fluid accumulation that creates swelling. Yet, many patients unknowingly become dehydrated during recovery due to difficulty drinking normally or concerns about disrupting blood clots. Maintaining proper fluid balance actually supports faster resolution of post-surgical inflammation.
How Dehydration Prolongs Swelling
Dehydration thickens your blood and makes it harder for your circulatory system to transport nutrients to healing tissues while removing inflammatory byproducts. This creates a cycle where poor hydration prolongs the inflammatory response, extending both swelling duration and overall recovery time.
Safe Ways to Stay Hydrated After Extraction
Water remains the best choice, but room temperature or slightly cool liquids cause less discomfort than ice-cold drinks during the first few days. Avoid straws completely, as suction can dislodge blood clots and trigger painful dry socket complications. Small, frequent sips work better than large gulps.
Electrolytes and Fluid Balance During Healing
Electrolyte balance matters too, especially if you are eating very little during early recovery. Clear broths, coconut water, or diluted sports drinks can help maintain proper sodium and potassium levels, supporting healthy fluid balance and reducing the body’s tendency to retain excess water in tissues.
Which Foods Can Help Manage Swelling Safely?
Your dietary choices during recovery directly influence inflammation levels and the rate of healing. Certain foods contain natural compounds that help reduce swelling, while others can actually worsen inflammation and prolong recovery. The challenge lies in choosing options that provide anti-inflammatory benefits while meeting the texture and temperature requirements of post-extraction healing.
Best Anti-Inflammatory Foods for Early Recovery
Anti-inflammatory foods that work well during early recovery include cold Greek yogurt enriched with probiotics, which supports immune function while providing protein for tissue repair. Smoothies made with berries, leafy greens, and protein powder deliver concentrated antioxidants that help control inflammation, though avoid using straws for consumption.
Cold soups like gazpacho or chilled cucumber soup provide hydration and nutrients while the cool temperature offers comfort to sore tissues. Bone broth served at room temperature provides collagen and minerals that support tissue healing, making it easy to consume when chewing remains difficult.
Natural Spices That Reduce Post-Surgical Swelling
Certain spices and herbs demonstrate measurable anti-inflammatory effects. Turmeric contains curcumin, which research shows can reduce post-surgical swelling when consumed regularly. Add small amounts to smoothies or warm (not hot) golden milk. Ginger offers similar benefits and can be consumed as a mild tea or added to soft foods.
Foods and Drinks to Avoid During the First Week
Foods to avoid during the first week include anything that requires significant chewing, as this can irritate extraction sites and increase swelling. Skip crunchy, spicy, or very hot foods that could irritate your tissues. Alcohol interferes with healing and can interact with pain medications, while excessive sugar can promote inflammation.
- Avoid chips, nuts, popcorn, and hard bread crusts.
- Skip chili, hot sauces, and heavily spiced curries.
- Do not drink alcohol or hot coffee for at least 72 hours.
- Limit candy, soda, and other high-sugar items.
- Avoid tomato-, citrus-, and vinegar-based foods, as they can sting wounds.
Nutritional Timing for Optimal Healing
Nutritional timing matters as much as food choices. Eat small, frequent meals rather than large portions. This approach maintains steady nutrition delivery to healing tissues without overwhelming your digestive system when you are likely moving and eating less than normal.
Professional consultation becomes particularly valuable when pre-existing conditions like diabetes affect healing, or when medications limit your food options. Working with an oral surgeon in Elizabeth ensures your dietary approach aligns with your specific surgical situation and medical history.
When Is Swelling a Sign of a Complication?
Normal post-extraction swelling follows predictable patterns that help distinguish routine healing from developing complications. Understanding these patterns prevents both unnecessary worry about normal symptoms and dangerous delays in seeking care for actual problems.
What Normal Swelling Looks Like
Expected swelling progression peaks between 48 and 72 hours, then steadily decreases over the following week. The affected area may feel firm, but should not be extremely painful to light touch. Skin color may show mild discoloration, but it should gradually improve rather than becoming more intense or spreading to new areas.
Warning Signs That Require Immediate Attention
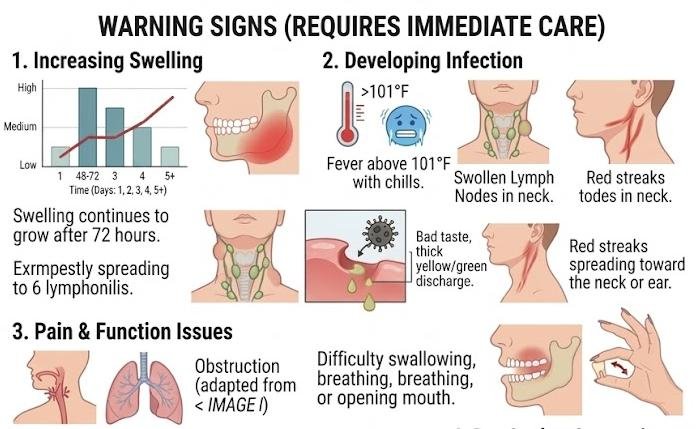
Warning signs requiring immediate attention include swelling that continues to increase after 72 hours, fever above 101 degrees Fahrenheit, severe pain that worsens rather than improves with prescribed medications, or difficulty swallowing or breathing. Red streaking extending from the extraction site toward your neck or ear indicates a possible spreading infection and requires urgent treatment.
- Swelling that keeps growing after day three.
- Fever above 101 degrees Fahrenheit with chills.
- Pain that worsens despite prescribed medication.
- Difficulty swallowing, breathing, or opening the mouth.
- Red streaks spreading toward the neck or ear.
Signs of Infection After Extraction
Infection symptoms often accompany problematic swelling and include persistent bad taste, thick yellow or green discharge from extraction sites, or swollen lymph nodes in your neck. Unlike normal post-surgical drainage, infected sites typically produce increasingly foul-smelling discharge and do not respond to routine care measures.
How Dry Socket Differs From Normal Swelling
Dry socket complications present differently, with severe pain typically developing 3 to 5 days after extraction rather than immediate swelling. However, some patients experience both conditions simultaneously, making professional evaluation crucial when symptoms do not follow expected patterns.
When to Contact Your Oral Surgeon
Geographic considerations matter for swelling assessment. Lower extractions typically cause more visible facial swelling, while upper extractions might affect the area under your eyes or around your sinuses. Swelling that extends significantly beyond the immediate extraction area or affects both sides of your face when only one side had surgery warrants professional evaluation.
Contact your oral surgeon if you are uncertain about any symptoms. Most practices maintain emergency contact protocols specifically for post-surgical concerns, and early intervention for complications prevents more serious problems that could require additional procedures or hospitalization.
How Can Preoperative Preparation Influence Swelling?
Pre-surgical preparation significantly impacts both swelling severity and overall recovery speed, yet many patients focus only on post-operative care. The days leading up to your extraction offer opportunities to optimize your body’s healing response and minimize the risk of inflammatory complications before they develop.
Nutritional Preparation Before Extraction
Nutritional preparation should begin at least a week before surgery. Focus on foods rich in vitamin C, which support collagen synthesis, essential for tissue repair. Increase protein intake to provide amino acids needed for healing, and ensure adequate zinc levels through foods like pumpkin seeds or lean meats, as zinc deficiency can impair wound healing and increase inflammation.
Lifestyle Changes That Support Faster Healing
Lifestyle modifications in the week before surgery make measurable differences in recovery outcomes. If you smoke, stopping at least 72 hours before surgery improves circulation and reduces infection risk. Even this brief cessation helps, though longer periods provide greater benefits. Limit alcohol consumption, which interferes with immune function and can interact with anesthesia or pain medications.
Oral Hygiene Steps Before the Procedure
Oral hygiene optimization reduces bacterial load around extraction sites, minimizing post-surgical infection risk and swelling. Use an antimicrobial mouthwash for several days before surgery, but stop the night before as directed by your surgeon. Thorough brushing and flossing in areas away from the surgical site helps maintain overall oral health during recovery when normal hygiene becomes challenging.
Sleep, Stress, and Immune Readiness
Sleep and stress management before surgery affect your immune system’s ability to handle the upcoming trauma. Aim for 7 to 8 hours of sleep nightly in the week leading up to extraction. High stress levels increase cortisol production, which can interfere with healing and potentially worsen inflammatory responses.
Medications and Supplements to Review
Medication planning involves understanding which supplements or medications might increase bleeding or interact with anesthesia. Stop taking fish oil, vitamin E, or other blood-thinning supplements as directed by your surgeon, typically 5 to 7 days before surgery. Arrange for prescription pain medications to be filled in advance so they are available immediately after your procedure.
Setting Up Your Recovery Space at Home
Recovery environment preparation includes organizing your post-surgical space with extra pillows for elevation, ice packs, and easy-to-prepare soft foods. Having everything ready before surgery reduces stress during early recovery, when decision-making can feel more difficult and moving around can be uncomfortable.
- Stack two to three pillows on the bed to elevate the head.
- Keep gel ice packs and a thin cloth barrier ready in the freezer.
- Stock yogurt, smoothie ingredients, broth, mashed potatoes, and eggs.
- Place prescribed medications, gauze, and water bottles within arm’s reach.
- Arrange a ride home and a helper for the first 24 hours.
The investment in thorough preparation pays dividends during recovery, often reducing both the intensity and duration of post-surgical swelling while setting the stage for optimal healing outcomes.
Final Conclusion
Managing swelling after wisdom teeth removal is less about fighting inflammation and more about guiding it. The first 72 hours set the tone for the entire recovery, which is why ice cycles, head elevation, careful hydration, and soft anti-inflammatory foods make such a noticeable difference when used consistently. Add thoughtful preparation in the week before surgery, including better nutrition, improved sleep and reduced smoking or alcohol use. The body walks into the procedure ready to heal rather than react.
The patients who recover fastest are rarely the ones who did one thing perfectly. They are the ones who stacked small, correct habits together. Use cold therapy properly, sleep propped up, sip water without a straw, choose Greek yogurt over chips, and watch closely for the warning signs that separate normal swelling from a complication. When anything feels off, call your oral surgeon rather than wait. With the right routine and realistic expectations, most people move from peak swelling to near-normal appearance within a week and return to full comfort shortly after.
Medical Disclaimer
The information in this article is provided for general educational purposes only and is not intended as a substitute for professional medical or dental advice, diagnosis, or treatment. Always consult your oral surgeon, dentist, or another qualified healthcare provider with any questions about wisdom teeth removal, post-surgical swelling, medications, or specific recovery concerns. Do not disregard or delay seeking professional advice because of something you have read here. Individual recovery experiences vary based on surgical complexity, age, overall health, and other factors, and the strategies described may not be appropriate for every patient. Any reliance on the information in this article is strictly at your own risk.
References
- American Association of Oral and Maxillofacial Surgeons. (2024). Wisdom Teeth Management Guidelines and Patient Recovery Statistics.
- Journal of Oral and Maxillofacial Surgery. (2023). Cold Therapy Protocols and Post-Extraction Edema: A Clinical Review.
- International Journal of Dentistry. (2022). Anti-Inflammatory Effects of Curcumin and Ginger in Post-Surgical Dental Recovery.
- British Journal of Oral and Maxillofacial Surgery. (2023). Risk Factors for Prolonged Swelling After Third Molar Extraction.
- American Dental Association. (2024). Patient Guidelines for Recovery After Tooth Extraction.
- Journal of Clinical Periodontology. (2022). Influence of Pre-Surgical Nutritional Status on Healing Outcomes in Oral Surgery.
- National Institutes of Health. (2023). Hydration, Lymphatic Function, and Post-Operative Recovery.
- Mayo Clinic. (2024). Dry Socket and Infection After Wisdom Teeth Removal: Clinical Overview.