Starting a new diabetes medication can feel uncertain. Victoza (liraglutide) is a once-daily injectable medication used primarily to improve blood sugar control in adults with type 2 diabetes. It belongs to a class of drugs called GLP-1 receptor agonists, which work by mimicking a natural hormone that stimulates insulin release, slows digestion, and reduces appetite.
The first month is the most important phase of Victoza treatment. This is when the body begins adapting to the medication, the dose is gradually increased, and most early side effects appear and typically resolve. Knowing what to expect during these four weeks helps patients stay consistent, manage discomfort confidently, and recognise genuine progress.
What Is Victoza (Liraglutide)?
Victoza is a brand name for liraglutide, a GLP-1 receptor agonist injected once daily using a pre-filled pen. It is prescribed for adults with type 2 diabetes to improve blood sugar control alongside diet and exercise. It is also used to reduce the risk of major cardiovascular events in people with type 2 diabetes and established heart disease. It is not insulin and is not approved as a first-line treatment for type 1 diabetes.
1. How Victoza Works in the Body
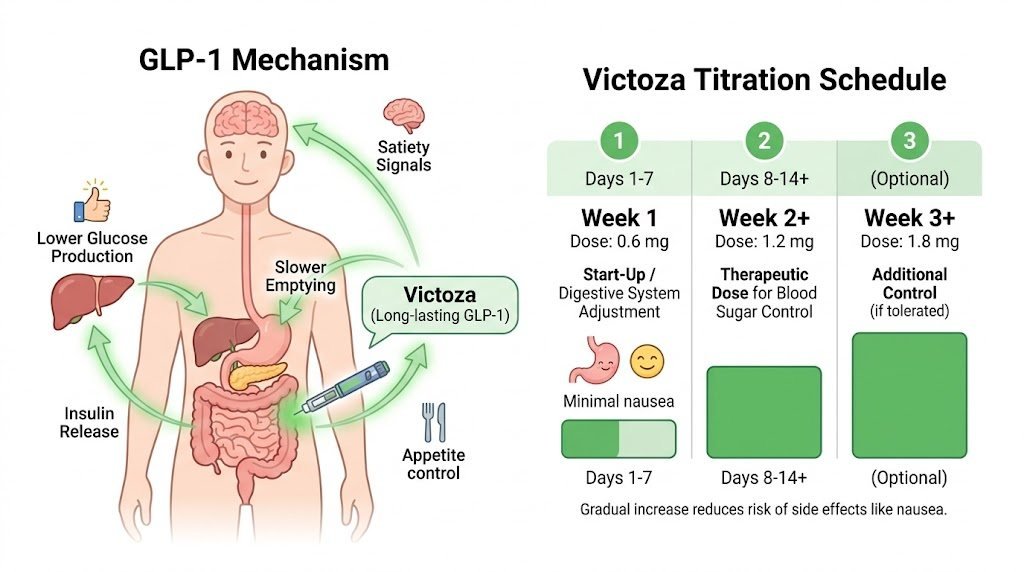
GLP-1 Mechanism Explained Simply
GLP-1 (glucagon-like peptide-1) is a hormone naturally released by the gut after eating. It signals the pancreas to release insulin when blood sugar rises, tells the liver to reduce glucose production, slows the rate at which food moves from the stomach into the small intestine, and sends satiety signals to the brain that reduce hunger.
Victoza mimics this hormone but with a much longer duration of action than the natural version. This means its effects on blood sugar regulation and appetite persist throughout the day from a single daily injection. The result is steadier blood sugar levels, reduced post-meal glucose spikes, and a generally reduced appetite that supports better portion control.
Why the First Month Is a Gradual Process
Victoza dosing follows a structured titration schedule. The treatment begins at a lower dose of 0.6 mg daily, which is below the therapeutic dose for blood sugar control. This starting dose exists purely to allow the digestive system to adjust, reducing the severity of early side effects such as nausea. The therapeutic Victoza dosing range begins at 1.2 mg daily, with some patients eventually moving to 1.8 mg daily if additional blood sugar control is needed and the lower dose is well tolerated.
Rushing this titration by increasing the dose too quickly significantly increases the risk of nausea, vomiting, and other gastrointestinal side effects. The structured approach is intentional and clinically important.
2. Week-by-Week Breakdown of the First Month
The following table gives a clear overview of what is typically happening medically and what patients commonly experience during each week of the first month.
| Week 1 | 0.6 mg once daily | Body begins adjusting; mild nausea or reduced appetite may appear | Mild digestive adjustment; energy may feel lower than usual |
| Week 2 | 0.6 mg once daily | Appetite control often becomes more noticeable; meal portions feel more satisfying | Nausea typically reduces; eating patterns begin to stabilise |
| Week 3 | 1.2 mg once daily (if tolerated) | Blood sugar fluctuations may begin to reduce; hunger cues become more regulated | Routines around dosing timing become easier to maintain |
| Week 4 | 1.2 mg once daily | Glucose control improves steadily; energy levels may begin to feel more consistent | Progress is gradual but measurable; body is adapting well |
Week 1: The Adjustment Begins
The first week begins with a 0.6 mg daily dose. At this level, Victoza is not yet working at full therapeutic capacity for blood sugar control, but the body is beginning to encounter the medication for the first time. This week is almost entirely about tolerance rather than treatment.
Most patients experience some degree of nausea during the first week, particularly in the hours after the injection. This is the most commonly reported early side effect and is caused by the slowing of gastric emptying that liraglutide produces. Eating smaller, lighter meals and avoiding high-fat or heavily spiced food helps significantly.
Appetite may also begin to decrease during the first week. Some patients find that meals feel more satisfying at a smaller volume. This is an early sign that the medication is functioning as intended.
Week 2: Patterns Begin to Emerge
By the second week, most patients report a reduction in nausea compared to the first week. The digestive system has begun adapting, and the medication is becoming more predictable. Appetite changes become more noticeable, with many patients reporting that they feel full more quickly and that food cravings are less frequent.
This is a good week to establish a consistent injection time. Taking Victoza at the same time each day, whether morning or evening, helps maintain steady drug levels in the body. The injection can be taken with or without food, but pairing it with an existing daily habit makes adherence significantly easier.
Week 3: Dose Increase if Tolerated
If the first two weeks have been tolerated without significant side effects, the prescribing doctor will typically increase the dose to 1.2 mg daily at the start of week three. This is the minimum therapeutic dose at which meaningful blood sugar improvements are expected.
Some patients experience a brief return of mild nausea when the dose increases. This is normal and usually passes within a few days. Using the same dietary strategies from week one (smaller meals, lighter foods, good hydration) helps manage this transition.
Blood sugar fluctuations may begin to reduce during this week. Patients who monitor their glucose at home may start to see post-meal readings that are lower and more consistent than before starting treatment.
Week 4: Settling Into a Routine
By the fourth week, most patients have moved through the main adjustment period. Nausea, if present at all, is typically mild and manageable. The dose is stable at 1.2 mg daily, and its effects on appetite regulation and blood sugar control are becoming consistent rather than variable.
Energy levels often begin to feel more stable during week four as blood sugar control improves. Many patients also find that their eating patterns have naturally shifted toward smaller, more regular meals without requiring significant conscious effort. This behavioural shift, supported by the appetite-regulating effects of the medication, is one of the key long-term benefits of GLP-1 treatment.
Progress Reminder:
It is important to understand that the first month of Victoza treatment is primarily an adjustment and tolerance phase. Significant improvements in HbA1c (long-term blood sugar marker) typically become measurable at the 8 to 12 week mark. Do not judge the effectiveness of the medication solely on how you feel during the first four weeks.
3. Early Physical Responses and How to Manage Them
Complete Side Effect Reference for the First Month
The following table covers the most commonly reported side effects during the first month of Victoza treatment, how frequently they typically occur, and practical steps to reduce their impact.
| Nausea after meals | Very common (up to 40% of users) | Eat smaller portions; avoid fatty or spicy foods; take dose at same time daily |
| Reduced appetite | Common; usually welcome | Eat nutritious smaller meals; do not skip meals entirely |
| Fatigue or low energy | Mild and temporary | Staying hydrated; maintain light activity; inform your doctor if it persists beyond week 2 |
| Bloating or wind | Mild and usually short-lived | Avoid carbonated drinks; eat slowly; reduce high-fibre foods temporarily |
| Diarrhoea or loose stools | Less common; usually resolves | Stay hydrated; inform your doctor if persistent beyond a few days |
| Injection site reactions | Mild redness or discomfort | Rotate injection sites; use room-temperature medication |
Side Effects That Require Immediate Medical Attention
While the side effects listed above are common and generally manageable, a small number of more serious reactions can occur. Contact your doctor or seek urgent medical attention if you experience any of the following:
- Severe and persistent abdominal pain that radiates to the back may indicate pancreatitis
- Signs of an allergic reaction include swelling of the face, lips, or throat, difficulty breathing, or a rapid heartbeat
- Symptoms of low blood sugar (hypoglycaemia), including shaking, sweating, confusion, or rapid heartbeat, particularly if taking Victoza alongside insulin or sulphonylureas
- Changes in vision or signs of kidney problems, including reduced urination or swelling in the legs
- A lump or swelling in the neck, hoarseness, or difficulty swallowing, which may rarely indicate thyroid changes
When to Contact Your Doctor:
Never attempt to manage severe or persistent side effects without medical guidance. If nausea or vomiting is severe enough to prevent you from eating or drinking, contact your prescribing team. Do not stop taking Victoza suddenly without medical advice, as this can affect your blood sugar control.
4. Appetite and Eating Pattern Changes

Why Appetite Decreases With Victoza
One of the most clinically significant effects of liraglutide is its impact on appetite regulation. GLP-1 receptors in the brain, particularly in the hypothalamus, respond to liraglutide by reducing hunger signals and increasing feelings of satiety. This effect operates independently of blood sugar levels, which is why appetite changes can be noticed even before meaningful glucose improvements occur.
Patients commonly describe meals as feeling satisfying at a smaller volume, a reduced desire for high-calorie or sweet foods, and a general reduction in the frequency of hunger throughout the day. These changes are not simply a side effect of nausea suppressing appetite. They represent a genuine shift in appetite-regulating signals that continues even after nausea resolves.
How to Eat Well During the First Month
The appetite changes that Victoza produces are most beneficial when supported by appropriate nutritional choices. Eating less is only helpful if what you eat still provides adequate protein, fibre, vitamins, and minerals. The following principles help patients get the most from their reduced appetite:
- Prioritise protein at every meal: Protein supports satiety, preserves muscle mass, and helps stabilise blood sugar. Eggs, fish, poultry, legumes, and Greek yoghurt are all practical choices.
- Do not skip meals: Even with reduced appetite, eating regular, small meals maintains steady blood sugar levels and prevents rebound hunger that can lead to poor food choices.
- Choose low-glycaemic carbohydrates: Wholegrains, vegetables, and legumes raise blood sugar more gradually than refined carbohydrates, supporting the blood sugar control that Victoza provides.
- Stay well hydrated: Adequate hydration supports digestion, reduces nausea, and helps the kidneys function well. Aim for at least 1.5 to 2 litres of water daily.
- Avoid eating through nausea: If nausea is present, eating smaller amounts more slowly rather than forcing a full meal helps reduce discomfort without compromising nutrition.
5. Dose Schedule and Building a Daily Routine
Standard Victoza Titration Schedule
The standard dosing schedule prescribed for most new Victoza users follows this structure:
- Weeks 1 and 2: 0.6 mg once daily (starter dose for tolerance, not full therapy)
- • After 4 or more weeks at 1.2 mg: increase to 1.8 mg daily only if additional blood sugar control is needed and the lower dose is tolerated
Your prescribing doctor may adjust this schedule based on your individual response, kidney function, and any other medications you are taking. Never change your dose without explicit instruction from your healthcare team.
Choosing Your Injection Time
Victoza can be injected at any time of day, independent of meals. The most important factor is consistency. Injecting at approximately the same time each day maintains steady drug levels in the bloodstream and makes adherence easier to sustain.
Common strategies that patients find helpful include:
- Injecting first thing in the morning alongside another daily habit, such as taking other medications or making breakfast
- Injecting in the evening as part of a wind-down routine, which some patients find reduces nausea by allowing it to pass during sleep
- Setting a phone alarm or using a medication reminder app for the first month until the habit is fully established
Correct Injection Technique
Using the correct technique reduces the risk of injection site reactions and ensures consistent medication delivery:
- Inject into the abdomen, upper thigh, or upper arm. The abdomen is most commonly used for its convenience and predictable absorption.
- Rotate injection sites within the same region to avoid lipohypertrophy (a hardening of tissue under the skin caused by repeated injections in the same spot).
- Allow the medication pen to reach room temperature before injecting if stored in the refrigerator. Cold medication increases the likelihood of injection site discomfort.
- Do not inject into skin that is tender, bruised, or hardened from previous injections.
- Dispose of needles safely in a sharps container. Never recap or reuse needles.
Medication Storage:
Victoza pens should be stored in the refrigerator between 2 and 8 degrees Celsius before first use. Once opened, the pen can be kept at room temperature (below 30 degrees Celsius) or refrigerated and used within 30 days. Never freeze Victoza. Do not use the medication if it has been frozen or if it appears cloudy or discoloured.
6. Medication Supply, Storage, and Treatment Consistency
Why Supply Consistency Matters in the First Month
Interruptions to Victoza treatment during the first month are particularly disruptive because the body is actively adapting to the medication. Missing doses during the titration phase can mean restarting the adjustment process, re-experiencing side effects that had already resolved, and losing early progress in blood sugar stabilisation.
Ensuring a consistent, uninterrupted supply of correctly stored medication is therefore a practical patient safety concern, not just a matter of convenience.
What to Look for in a Verified Medication Supplier
For patients obtaining Victoza through pharmacy or licensed online dispensing services, the following standards are important to verify:
- Temperature-controlled storage and delivery: Liraglutide is sensitive to temperature and must remain refrigerated throughout the supply chain until dispensed.
- Licensed dispensing: ensure any pharmacy or dispensing service is registered with the relevant regulatory body, such as the General Pharmaceutical Council (GPhC) in the UK or the relevant state board of pharmacy in the US.
- Clear labelling and patient information: verified dispensers provide manufacturer packaging, accurate expiry dates, and patient information leaflets.
- Regulated fulfilment: avoid unlicensed online sources that offer Victoza at significantly discounted prices without requiring a valid prescription. These sources carry genuine risks of counterfeit or improperly stored medication.
Important Supply Warning:
Counterfeit GLP-1 medications have been reported in multiple countries. Always obtain Victoza through a licensed pharmacy or a healthcare provider. If your medication looks different from what you have previously received, do not use it and contact your pharmacist or prescribing doctor immediately.
7. What Progress Looks Like in the First Month
Realistic Expectations for the First Four Weeks
One of the most common sources of frustration during the first month of Victoza treatment is expecting changes that are not typical at this stage. Understanding what is and is not realistic helps patients stay motivated and interpret early results accurately.
Blood Sugar Changes
At the 1.2 mg therapeutic dose, meaningful improvements in fasting blood glucose and post-meal readings typically begin to emerge during weeks three and four. The most clinically significant measure, HbA1c (a measure of average blood sugar over approximately three months), will not reflect first-month progress on a blood test. Meaningful HbA1c changes are typically visible at the 3-month review.
Weight Changes
Weight loss during the first month is usually modest, typically ranging from 1 to 3 kilograms in patients who experience meaningful appetite suppression. The primary weight-related benefit of Victoza is not a rapid short-term reduction but a gradual, sustained reduction over months of treatment supported by the medication’s appetite-regulating effects. Expecting significant weight loss in the first four weeks sets an unrealistic benchmark.
Energy and Wellbeing
Improved energy is one of the benefits patients notice first when blood sugar regulation begins to improve. Consistently high blood sugar causes fatigue, poor concentration, and low mood. As Victoza reduces post-meal glucose spikes and stabilises fasting glucose, many patients report feeling more consistently alert and less prone to afternoon energy crashes by the end of the first month.
Signs That Treatment Is Working
- • Post-meal blood glucose readings are lower and more consistent than before starting Victoza
- Appetite is noticeably reduced, and meals feel satisfying at a smaller volume
- Energy levels feel more stable throughout the day
- Nausea and other early side effects have reduced significantly from week one
- The daily injection routine has become established and manageable
Tracking Tip:
Keep a simple daily log during the first month, recording your fasting blood glucose reading each morning, your injection time, any side effects and their severity, and your general energy level on a scale of 1 to 10. This log is valuable to share with your diabetes care team at your first follow-up appointment and helps identify patterns that would otherwise be easy to miss.
Frequently Asked Questions
Can I inject Victoza at a different time than usual if I forget?
- If you miss a dose and it is within 12 hours of your usual injection time, take it as soon as you remember. If more than 12 hours have passed since your scheduled dose, skip it and resume your normal schedule the following day. Never take two doses in one day to make up for a missed dose.
Is it normal to still feel nauseous in week three or four?
- Some degree of nausea during week three is common, particularly if the dose has just been increased from 0.6 mg to 1.2 mg. However, persistent severe nausea beyond the first two weeks at any dose warrants a conversation with your prescribing doctor. They may recommend delaying the dose increase or adjusting your injection timing.
Will Victoza interact with other medications I am taking?
- Victoza can interact with several medications. It slows gastric emptying, which can affect the absorption rate of oral medications taken at the same time. It also increases the risk of low blood sugar when combined with insulin or sulphonylureas. Always provide your full medication list to your prescribing doctor and pharmacist before starting Victoza.
How should I store my Victoza pen once I have opened it?
- Once opened, a Victoza pen can be stored at room temperature below 30 degrees Celsius or in the refrigerator. It must be used within 30 days of first use. Never freeze the pen. Always attach a new needle immediately before each injection and remove it afterwards. Do not store the pen with the needle attached.
What should I do if I experience severe stomach pain?
- Severe abdominal pain, particularly pain that spreads to the back and is accompanied by nausea and vomiting, can be a sign of pancreatitis, a rare but serious complication associated with GLP-1 receptor agonists. Stop taking Victoza and seek immediate medical attention if you experience these symptoms.
Can I drink alcohol while taking Victoza?
Alcohol can affect blood sugar levels and may increase the risk of hypoglycaemia, particularly in patients also taking insulin or sulphonylureas. Moderate alcohol consumption is generally considered acceptable, but discuss your specific circumstances with your diabetes care team. Avoid drinking on an empty stomach.
Disclaimer
This article has been prepared for general informational and educational purposes only. Doctiplus and its contributors do not provide medical advice, diagnosis, or treatment recommendations. Victoza is a prescription-only medication. The information in this article does not replace the guidance of your prescribing doctor, diabetes specialist nurse, or pharmacist. Always follow the specific instructions provided by your healthcare team regarding dosing, storage, and management of side effects. If you have concerns about your medication or experience unexpected symptoms, contact your healthcare provider promptly.

