According to the American Society for Reproductive Medicine, approximately 12% of women of reproductive age experience infertility yet the number of egg donation cycles performed annually has grown by over 40% since 2015. As fertility treatments become more sophisticated and culturally accepted, egg donation has emerged as a critical path for thousands of families who cannot conceive using their own genetic material. The process involves far more than a simple medical procedure; it’s a months-long journey that demands significant commitment from donors and careful coordination between medical teams, psychological counselors, and legal professionals.
- For potential donors, understanding this timeline means making an informed decision about a process that will impact several months of their lives.
- For intended parents, it provides realistic expectations about when treatment might begin and what coordination is required.
- The journey from initial application to final recovery involves multiple phases of screening, preparation, and medical intervention each with its own requirements and considerations that extend well beyond the day of egg retrieval itself.
What Happens Step by Step in the Egg Donation Process
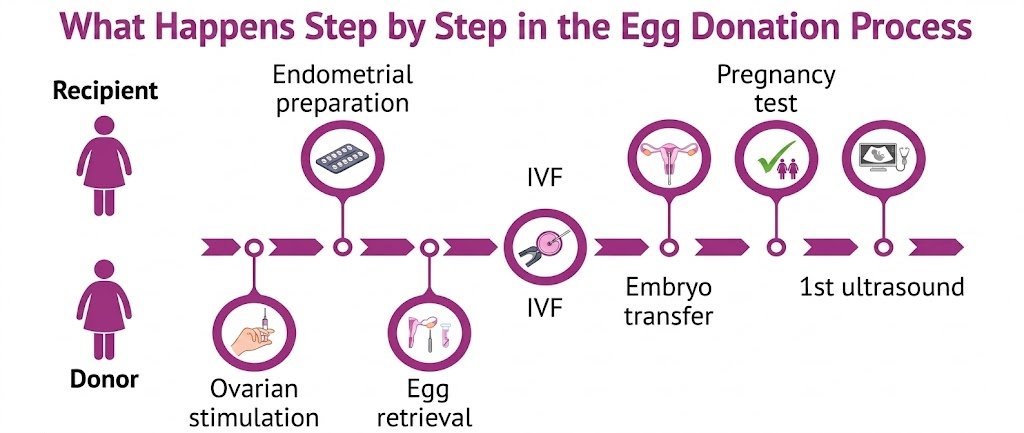
The egg donation timeline typically spans 3-6 months from initial application to recovery, though this varies based on clinic protocols and individual circumstances. The journey begins with an extensive application process where potential donors complete detailed questionnaires covering family medical history, lifestyle factors, educational background, and personal motivations. This initial phase can take 2-4 weeks as clinics review applications against their specific criteria.
Once accepted into a program, donors enter a comprehensive screening phase lasting 4-8 weeks. This involves multiple clinic visits for medical testing, psychological evaluation, and genetic counseling. During this period, many donors are also matched with intended parents a process that can happen quickly or take several weeks depending on preferences and availability.
The active treatment cycle begins once all parties are ready and synchronized. Donors start birth control pills to regulate their cycle, followed by 2-3 weeks of hormone injections to stimulate egg production. Daily monitoring through blood work and ultrasounds becomes routine during stimulation, requiring donors to visit the clinic every other day, then daily as retrieval approaches.
Egg retrieval occurs approximately 10-14 days after stimulation begins, performed under light sedation as an outpatient procedure. The entire medical intervention takes about 20-30 minutes, followed by 1-2 hours of recovery at the clinic. Most donors resume normal activities within 24-48 hours, though some experience bloating or discomfort for up to a week.
The final phase involves follow-up care, including a post-retrieval check within one week and final blood work to ensure hormone levels return to normal. This comprehensive timeline helps explain why successful egg donation requires significant planning and flexibility from all parties involved.
How Medical and Psychological Screening Prepares Donors
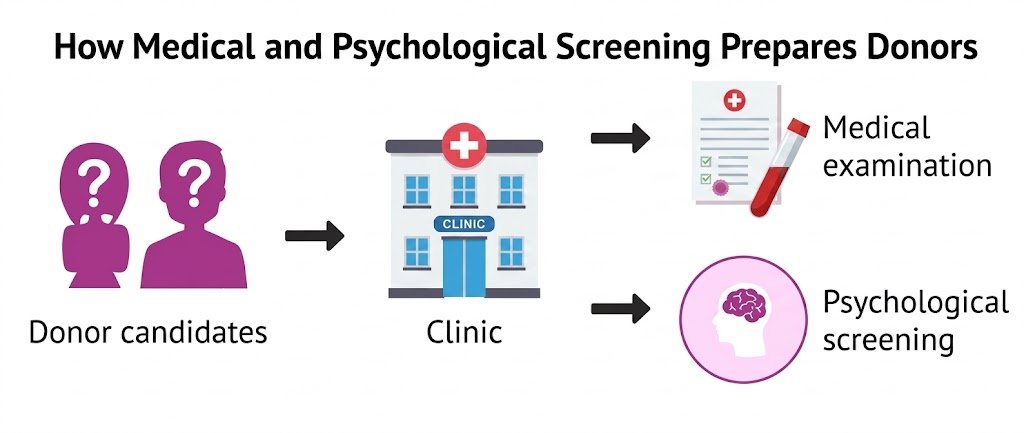
The screening process serves as both a safeguard and preparation phase, ensuring donors understand the commitment while protecting their health throughout the process. This dual evaluation addresses both physical readiness and psychological preparedness for an experience that many underestimate in its complexity.
What Medical Tests and Evaluations Are Required
Medical screening begins with comprehensive blood work testing hormone levels, infectious diseases including HIV and hepatitis, and genetic markers for inherited conditions. Donors undergo pelvic examinations, transvaginal ultrasounds to assess ovarian function, and sometimes additional testing like electrocardiograms depending on age and medical history. The FDA requires specific infectious disease testing within 30 days of egg retrieval, often necessitating repeated blood draws throughout the process.
Most programs require donors to be between ages 21-29, with some accepting candidates up to 30. Height and weight requirements exist, typically requiring a BMI between 18-28, though this varies by clinic. Donors must demonstrate regular menstrual cycles and cannot have used Depo-Provera injections within the past year, as this can affect ovarian response to stimulation medications.
Family medical history receives intense scrutiny, with many programs excluding donors whose immediate family members have histories of certain cancers, psychiatric conditions, or genetic disorders. Some clinics require donors to abstain from alcohol, tobacco, and recreational drugs for the duration of their participation, with random testing to verify compliance.
Why Psychological Screening Matters for Donors
Psychological evaluation involves meeting with a mental health professional who assesses emotional readiness, understanding of the process, and ability to cope with potential outcomes. Many donors enter screening without fully considering scenarios like what happens if intended parents experience pregnancy loss, or how they might feel seeing children who are genetically related to them.
The screening addresses practical concerns too: Can donors handle the stress of daily injections and frequent clinic visits? How will they manage if work schedules conflict with monitoring appointments? Do they have adequate support systems for the physical and emotional demands of the process? Counselors also ensure donors understand the legal implications of relinquishing parental rights and explore their feelings about anonymity versus contact with recipient families.
This evaluation isn’t designed to exclude people but to prepare them realistically. Many first-time donors underestimate the emotional weight of contributing to another family’s journey, particularly if previous attempts have failed. The psychological screening helps identify potential challenges early, often leading to additional counseling resources rather than disqualification. For those in Connecticut considering this path, understanding specific egg donor requirements in Connecticut helps clarify state-specific guidelines alongside these universal psychological considerations.
What to Expect During Egg Retrieval and Recovery
The actual egg retrieval represents the culmination of weeks of preparation, but the physical demands of ovarian stimulation often surprise donors who expect the process to feel more routine. Hormone injections typically begin with birth control pills to synchronize cycles, followed by daily subcutaneous injections of follicle-stimulating hormone (FSH) and luteinizing hormone (LH) for 8-12 days.
As follicles develop, donors experience noticeable physical changes. Ovaries can double or triple in size, causing bloating, abdominal pressure, and sometimes discomfort during normal activities like exercise or bending over. Monitoring appointments become daily affairs in the final week, requiring blood draws before dawn so results are available for same-day medication adjustments. This intense monitoring phase demands significant schedule flexibility, as retrieval timing cannot be predicted precisely.
The retrieval procedure itself involves transvaginal ultrasound guidance while a reproductive endocrinologist uses a thin needle to aspirate eggs from each follicle. Most clinics use conscious sedation, meaning donors remain drowsy but responsive throughout the 15-30 minute procedure. The number of eggs retrieved varies dramatically anywhere from 5-30 eggs is considered normal, with averages typically falling between 12-18 eggs per cycle.
Recovery involves monitoring for ovarian hyperstimulation syndrome (OHSS), a potentially serious condition where ovaries become severely enlarged and fluid accumulates in the abdomen. Mild OHSS affects up to 20% of donors, causing bloating and discomfort for several days. Severe cases requiring hospitalization are rare but possible, particularly in donors who produce high numbers of eggs.
Most donors resume normal activities within 2-3 days, though some experience fatigue or mood changes as hormone levels normalize over the following week. Heavy lifting and vigorous exercise are typically restricted for one week post-retrieval. The clinic monitors recovery through follow-up appointments and blood work to ensure complications don’t develop after discharge.
What Legal and Ethical Issues Affect Egg Donation
Egg donation exists within a complex framework of state and federal regulations, with significant variations in laws governing anonymity, compensation, and parental rights. Unlike other medical procedures, egg donation creates lasting legal relationships and obligations that extend far beyond the medical treatment itself.
Informed consent documents typically span dozens of pages, covering everything from medical risks to psychological implications to financial arrangements. These contracts establish that donors relinquish all parental rights and responsibilities for any children conceived using their eggs. However, the enforceability of these agreements varies by state, and some jurisdictions have yet to fully address scenarios involving donor-conceived children seeking biological information or contact.
Compensation practices differ dramatically across programs and states. While the American Society for Reproductive Medicine suggests reasonable compensation should range from $5,000-$10,000 per cycle, some programs offer significantly more for donors with specific characteristics. This variation raises ethical questions about potential exploitation and whether higher payments might pressure women to accept medical risks they wouldn’t otherwise consider.
Anonymity policies continue evolving as donor-conceived individuals increasingly seek biological family connections through DNA testing services. Many programs that once promised permanent anonymity now acknowledge this cannot be guaranteed in the digital age. Some clinics have moved toward “open” donation models where contact between parties is possible, though this remains less common in the United States compared to other countries.
The psychological welfare of all parties receives increased attention as the field matures. Professional organizations now emphasize the importance of ongoing counseling resources and recommend long-term support systems for donors, recipients, and donor-conceived children. These ethical considerations influence program policies and suggest the field will continue evolving as more research emerges about long-term outcomes for everyone involved in the donation process.
Understanding these legal and ethical complexities helps potential donors make informed decisions about participation while highlighting why thorough counseling and legal consultation remain essential components of responsible egg donation programs. The landscape continues shifting as technology, social attitudes, and legal frameworks adapt to the realities of modern reproductive medicine.
High Authority research References
- https://pubmed.ncbi.nlm.nih.gov/37347350/
- https://pubmed.ncbi.nlm.nih.gov/33742206/
- https://rbej.biomedcentral.com/articles/10.1186/s12958-025-01418-8
- https://bmcwomenshealth.biomedcentral.com/articles/10.1186/s12905-024-03302-w
- https://reproductive-health-journal.biomedcentral.com/articles/10.1186/s12978-024-01804-2
- https://pmc.ncbi.nlm.nih.gov/articles/PMC12579783/
- https://pubmed.ncbi.nlm.nih.gov/2673841/
- https://academic.oup.com/humupd/article/22/4/450/2573576
- https://www.dovepress.com/egg-donation-compensation-ethical-and-legal-challenges-peer-reviewed-fulltext-article-MB
- https://www.nature.com/articles/s41599-025-05755-2

