According to the American Dental Association’s 2023 practice survey, the average cost of a three-unit dental bridge ranges from $1,500 to $6,000 a price variation so wide it leaves many patients wondering what actually drives these differences. As dental technology advances and material options expand, the gap between basic and premium bridge solutions continues to widen, making cost transparency more crucial than ever.
This pricing uncertainty affects millions of Americans facing tooth loss, particularly as dental insurance coverage varies dramatically between plans and many procedures require significant out-of-pocket expenses. Understanding the specific factors that influence bridge costs from materials and location in the mouth to the complexity of fabrication becomes essential for making informed decisions about oral health investments.
For anyone considering a dental bridge, the challenge isn’t just finding an affordable option, but understanding which variables matter most and how different choices affect both immediate costs and long-term value. The decisions made during the treatment planning phase often determine whether a bridge represents excellent value or an expensive compromise.
What Factors Influence the Cost of a Dental Bridge
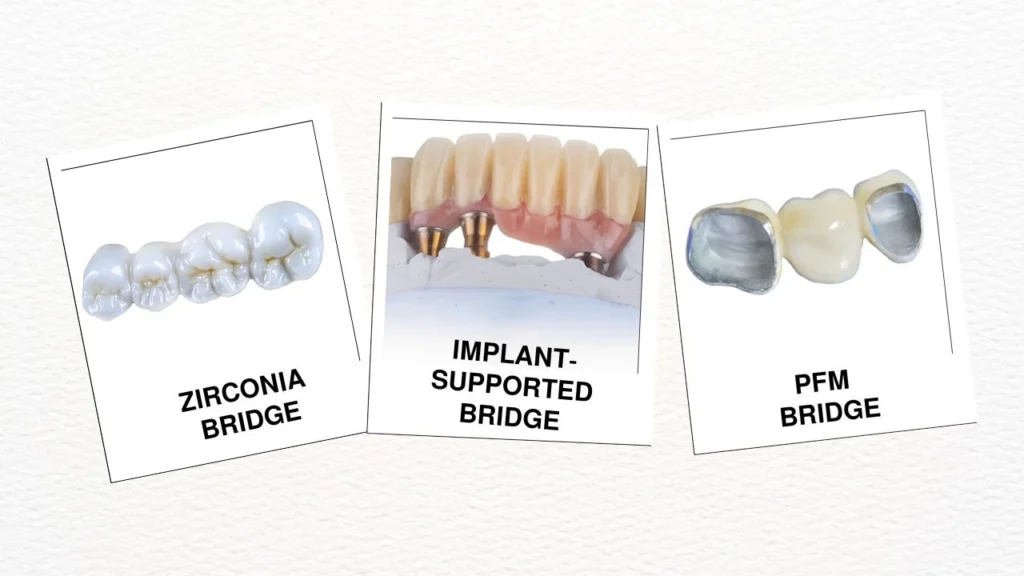
The most significant cost driver in dental bridge treatment is material selection, with options ranging from basic metal alloys to premium zirconia that can triple the price. Porcelain-fused-to-metal bridges typically fall in the middle range, while all-ceramic and zirconia options command premium pricing due to their superior aesthetics and biocompatibility. The manufacturing process for these advanced materials requires specialized equipment and expertise, directly impacting the final cost.
Location in the mouth creates another major pricing variable. Front teeth bridges often cost more due to heightened aesthetic requirements — the materials must match natural tooth color precisely, and the fabrication process demands greater attention to detail. Posterior bridges, while potentially requiring stronger materials to withstand chewing forces, may use less expensive options since appearance is secondary to function.
The number of units in a bridge affects cost in a non-linear fashion. A three-unit bridge doesn’t simply cost 50% more than a two-unit bridge because the abutment tooth preparation, impression procedures, and laboratory coordination remain largely the same regardless of span length. However, bridges spanning more than four teeth require additional engineering considerations and stronger materials, driving costs higher.
Preparatory work significantly influences the total investment. Teeth requiring root canal therapy, crown lengthening, or bone grafting before bridge placement can add $500 to $3,000 per tooth to the overall treatment cost. The condition of the abutment teeth — those supporting the bridge — determines whether simple preparation suffices or extensive restoration becomes necessary.
Geographic location and practice overhead create the final major cost variable. Urban practices with higher rent and labor costs typically charge 20-40% more than rural counterparts, while specialist prosthodontists command premium fees compared to general dentists performing the same procedures.
How Different Types of Dental Bridges Affect Cost
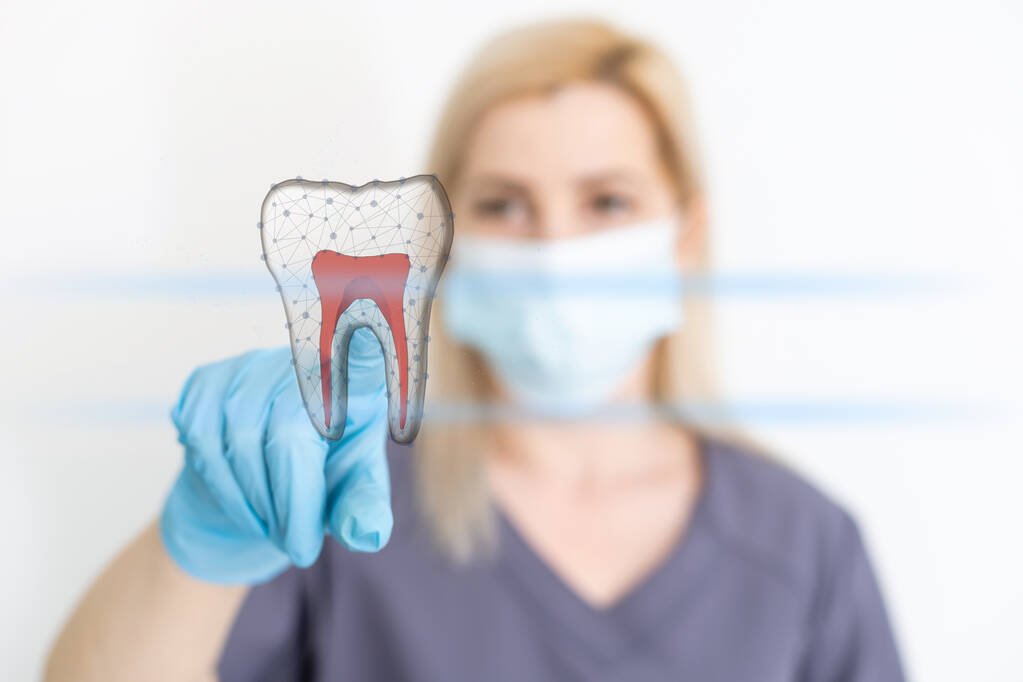
Traditional fixed bridges represent the most common and cost-effective solution for most patients, with prices typically ranging from $1,500 to $4,500 for a three-unit restoration. These bridges rely on crowns placed over adjacent teeth for support, making them suitable for patients with healthy teeth on either side of the gap. The straightforward design keeps laboratory costs reasonable while providing reliable long-term function.
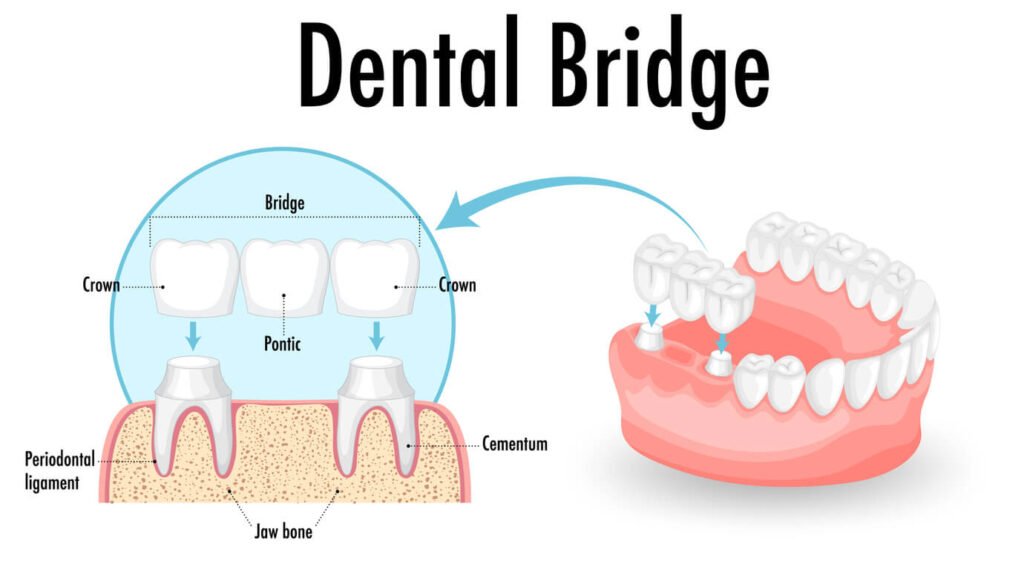
Implant-supported bridges command significantly higher fees often $6,000 to $15,000 for a three-unit span but eliminate the need to modify healthy adjacent teeth. The implant placement procedure adds surgical complexity and healing time, while the specialized abutments and connections increase material costs. However, this approach preserves natural tooth structure and may prove more economical over decades of use.
Maryland or resin-bonded bridges offer the most conservative approach, typically costing $1,000 to $2,500 for anterior applications. These bridges use metal or ceramic frameworks bonded to the back surfaces of adjacent teeth, requiring minimal tooth preparation. While initially less expensive, their limited durability and higher failure rates may necessitate replacement sooner than conventional bridges.
Comparing Bridge Materials and Their Prices
Porcelain-fused-to-metal (PFM) bridges balance cost and performance effectively, typically adding $200 to $500 per unit compared to basic metal options. The metal substructure provides strength while the porcelain overlay delivers acceptable aesthetics for most situations. However, the metal margin may become visible over time, particularly problematic for front teeth.
All-ceramic and zirconia bridges represent premium options, often costing $400 to $800 more per unit than PFM alternatives. Zirconia’s exceptional strength allows for thinner restorations while maintaining durability, and its tooth-like color eliminates the dark lines associated with metal-based bridges. The specialized milling equipment required for zirconia fabrication contributes to higher laboratory fees.
The investment in premium materials often proves worthwhile for front teeth, where the superior aesthetics justify additional cost. For posterior bridges, the strength advantages of zirconia may outweigh the price difference, particularly for patients with heavy bite forces or grinding habits.
Cost Considerations for Fixed vs Removable Bridges
Fixed bridges require higher upfront investment but eliminate daily removal and cleaning routines. The permanent attachment provides superior chewing function and prevents the bone loss associated with removable appliances. While initial costs run higher, fixed bridges typically last 10-15 years with proper care, making them cost-effective long-term solutions.
Removable partial dentures offer lower initial costs often $500 to $2,000 but require replacement every 5-7 years as the supporting tissues change. The clasps and framework may stress remaining teeth, potentially necessitating additional dental work over time. When considering lifetime costs, removable options may prove more expensive despite lower initial fees.
How Dental Bridges Are Made and Installed
The bridge fabrication process begins with precise tooth preparation, where the dentist removes a specific amount of tooth structure from the abutment teeth to accommodate crown thickness. This preparation must balance providing adequate space for durable materials while preserving maximum healthy tooth structure. The precision required for proper fit adds to chair time and influences overall treatment cost.
Digital impressions have largely replaced traditional putty molds in modern practices, improving accuracy while reducing patient discomfort. The specialized scanning equipment represents a significant practice investment, reflected in treatment fees. However, digital workflows often reduce the number of appointments required and eliminate remakes due to poor impressions, potentially offsetting higher initial costs.
Laboratory fabrication typically requires 10-14 days and involves skilled technicians working with precision equipment. The laboratory must create a restoration that matches the patient’s bite, provides proper contacts with adjacent teeth, and delivers appropriate aesthetics. Premium laboratories with advanced CAD/CAM technology and experienced ceramists charge higher fees but typically produce superior results.
The final installation appointment involves precise adjustments to ensure proper fit, bite, and comfort. This process cannot be rushed — improper adjustments can lead to bite problems, discomfort, or premature failure. The time investment required for proper delivery contributes to the overall treatment cost but proves essential for long-term success.
Temporary bridges worn during the fabrication period require additional materials and appointments, adding $200 to $500 to total treatment costs. However, these temporaries protect prepared teeth and maintain function and appearance during the waiting period.
Maintenance and Lifespan of Dental Bridges Affect Long-Term Costs
Proper daily hygiene requires specialized tools and techniques that add ongoing costs but dramatically extend bridge lifespan. Floss threaders, water flossers, and interdental brushes become essential for cleaning under the bridge pontic and around abutment teeth. Patients who invest $50-100 annually in proper cleaning tools often achieve 15+ years of bridge life, while those using only regular toothbrushes may face replacement within 8-10 years.
Professional maintenance includes regular cleanings every 3-4 months and periodic examinations to detect problems early. Many dental practices recommend specialized cleaning protocols for bridge patients, which may involve additional fees but help prevent the costly complications that lead to bridge failure. The investment in preventive care — typically $400-600 annually — proves minimal compared to bridge replacement costs.
Common failure modes include decay at the margins, abutment tooth fracture, and loss of retention. Margin decay often results from inadequate home care and can necessitate complete bridge replacement if extensive. When patients maintain excellent oral hygiene and avoid habits like ice chewing or using teeth as tools, bridges routinely last 12-15 years or longer.
The decision to restore missing teeth with a bridge represents a significant investment in both immediate comfort and long-term oral health, particularly when considering how untreated tooth loss affects adjacent teeth and overall bite stability. Understanding maintenance requirements upfront helps patients budget for the total cost of ownership rather than just initial treatment fees.
Insurance coverage typically provides 50% reimbursement for bridge treatment after deductibles, but annual maximums often limit total benefits to $1,500-2,500. Patients should factor insurance timing and benefit coordination into treatment planning, as splitting treatment across calendar years may maximize coverage.
How Do Dental Bridge Costs Compare with Dental Implants
Initial cost comparison favors bridges, with three-unit bridges typically costing $2,000-4,000 less than implant-supported alternatives. However, this comparison becomes complex when factoring in the need to crown healthy adjacent teeth for bridge support versus preserving those teeth with implants. The long-term value equation shifts when considering that bridges may require replacement while implants often last decades.
Lifetime cost analysis reveals surprising economics. A bridge replaced once after 12-15 years costs approximately the same as initial implant treatment, while the implant continues providing service. Additionally, bridge failure may compromise the supporting teeth, potentially requiring more extensive treatment. Implants eliminate this risk by standing independently.
Treatment timeline differences affect both cost and convenience. Bridges can often be completed within 2-3 weeks, allowing faster return to normal function. Implant treatment may require 3-6 months for healing, during which temporary solutions add cost and inconvenience. For patients needing immediate results, bridges provide clear advantages despite higher long-term costs.
Insurance coverage variations typically favor bridge treatment, with most plans providing standard coverage while classifying implants as optional or cosmetic procedures. This coverage difference can create $2,000-4,000 in out-of-pocket cost variation, making bridges more accessible despite potentially higher lifetime expenses.
The choice between bridges and implants ultimately depends on individual circumstances, timeline requirements, and financial priorities. Patients prioritizing immediate function and lower upfront costs often choose bridges, while those focused on long-term value and tooth preservation lean toward implants. Understanding both approaches helps ensure decisions align with personal needs and financial capabilities rather than simply choosing the lowest initial price option.