Weight-loss treatment is no longer a single-lane decision between “try harder with diet and exercise” and “have surgery.”
For adults living with obesity or weight-related metabolic concerns, the options now include physician-led endoscopic procedures that sit somewhere between those two extremes.
One of the most talked-about among them is endoscopic sleeve gastroplasty (ESG). It is often described as a non-surgical, incision-free weight-loss procedure, but that shorthand does not fully answer the question most patients actually have:
How does it compare to gastric sleeve surgery, and who is it really for?
That comparison matters. Both procedures aim to reduce stomach capacity and support meaningful weight loss. But they differ in how they are performed, how invasive they are, the expected recovery, and the amount of weight loss typically seen over time.
For patients trying to choose the right next step, understanding those differences is more useful than simply hearing that one is “less invasive” than the other.
What is endoscopic sleeve gastroplasty?
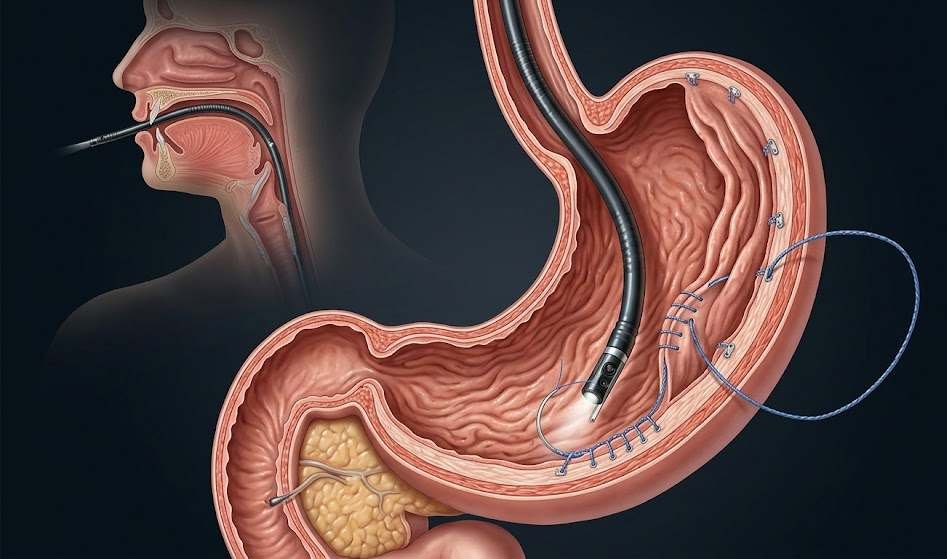
Endoscopic sleeve gastroplasty is a bariatric endoscopy procedure performed through the mouth using a flexible endoscope fitted with a suturing device. There are no cuts on the outside of the abdomen.
During the procedure, the doctor places a series of full-thickness sutures inside the stomach to reduce its size and change its shape into a narrower sleeve-like tube.
The result is a smaller stomach that holds less food and empties more slowly, which can help patients feel full sooner and stay full longer.
Because ESG is performed endoscopically rather than laparoscopically, it is generally considered less invasive than bariatric surgery.
Mayo Clinic notes that it may be an option for adults with a BMI of 30 or above when diet and exercise alone have not produced sufficient results. At the same time, the American Society for Metabolic and Bariatric Surgery says ESG should be offered as part of a comprehensive, multidisciplinary obesity treatment program for carefully selected patients.
And, because ESG is performed endoscopically rather than laparoscopically, it is generally considered less invasive than bariatric surgery. It may be an option for adults with a BMI of 30 or above when diet and exercise alone have not produced sufficient results, particularly when offered as part of a comprehensive obesity-care programme.
For patients moving from online research into a real clinical decision, the quality of the care model matters as much as the procedure itself. Everself is one example of a physician-led programme built around personalised obesity care, with support that includes eligibility assessment, nutrition counselling, and follow-up after treatment.
Its presence in states including Texas, Florida, and North Carolina also signals a broader, established approach rather than a one-off treatment offering. For readers exploring care locally, a sensible next step may be to book endoscopic sleeve gastroplasty in Charlotte, NC, through such a programme that provides this kind of end-to-end support.
What is gastric sleeve surgery?
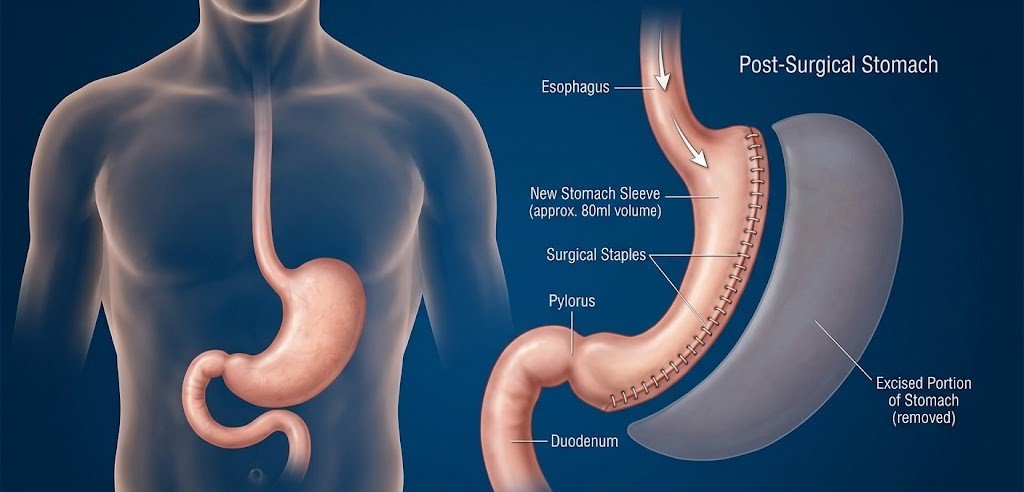
Gastric sleeve surgery, also called sleeve gastrectomy or laparoscopic sleeve gastrectomy, is a surgical bariatric procedure. Instead of placing sutures from inside the stomach, the surgeon removes most of the stomach permanently, leaving behind a narrow tube or “sleeve.”
This reduces how much food the stomach can hold and also affects gastrointestinal hormones that influence hunger, satiety, and metabolism.
Unlike ESG, gastric sleeve surgery involves abdominal incisions, general anesthesia, and the permanent removal of part of the stomach. It is one of the most established bariatric operations worldwide and is typically considered for patients with more severe obesity or obesity-related complications, depending on BMI and clinical profile.
NIDDK states that weight-loss surgery is generally considered for adults with a BMI of 40 or more, or 35 or more with a serious obesity-related condition. However, some patients with lower BMI may qualify in selected cases.
How ESG works in the body
From a patient perspective, ESG is not simply a “smaller stomach” procedure. It changes eating mechanics in several ways.
- First, reducing the stomach’s volume means meals need to be smaller.
- Second, the altered shape of the stomach slows gastric emptying, which can increase fullness after eating.
- Third, because ESG is usually delivered within a structured obesity-care program, it is typically combined with nutrition counseling, follow-up visits, and behavior change support rather than treated as a standalone fix.
This is important because the best outcomes in obesity care rarely come from anatomy alone. The procedure changes the physical environment of eating, but long-term success still depends on how well that change is supported with dietary guidance, monitoring, and realistic habit work.
ESG vs gastric sleeve surgery: the core differences
1. Procedure type
The biggest difference is procedural.
ESG is endoscopic. It is done through the mouth, without external incisions, and uses sutures to reduce stomach size from the inside. The gastric sleeve is surgical. It requires abdominal access, usually laparoscopic, and removes a large section of the stomach permanently.
2. Invasiveness and recovery
Because ESG avoids abdominal surgery, it is generally associated with a quicker return to daily activities and fewer scars.
The treatment is minimally invasive and notes a quick return to usual routines for many patients. Gastric sleeve surgery, while commonly performed and effective, is still a major operation and usually involves a more substantial recovery period. ClinicSpots’ own gastric sleeve overview for Turkey, for example, describes recovery on the scale of weeks rather than days.
That does not mean ESG is “easy” or free of side effects. Patients may still experience nausea, abdominal discomfort, dietary restrictions, and the need for close follow-up in the early phase. But the absence of incisions and overnight hospitalization often makes it attractive to people who want a less invasive option.
3. Expected weight loss
This is the point where many patient decisions become clearer.
In general, gastric sleeve surgery tends to produce more weight loss than ESG in the short to medium term. JAMA’s patient page on sleeve gastrectomy states that sleeve surgery can help patients lose more than 20% of total body weight in about a year. ESG outcomes are also clinically meaningful, but usually lower. Published long-term data suggest total body weight loss after ESG often falls in the mid-teens, with durable results reported at 5 years in many patients.
So the trade-off is straightforward: gastric sleeve usually offers greater weight-loss power, while ESG offers a less invasive route with meaningful, but typically more modest, results.
4. Reversibility and anatomy
Gastric sleeve surgery is permanent because part of the stomach is removed. ESG does not remove the stomach; it reshapes it internally with sutures. That distinction matters to patients who are not ready for irreversible surgery or who want to explore an earlier procedural intervention before moving to an operation.
5. Patient eligibility
Eligibility is not identical. ESG is often discussed for adults with obesity who may not meet, want, or qualify for bariatric surgery but still need more support than lifestyle change alone. Gastric sleeve is typically reserved for higher-BMI or more medically complex cases, although exact criteria vary by provider, country, and comorbidity profile.
Who may be a good candidate for ESG?
ESG may be worth discussing with a physician if:
- Your BMI is in the obesity range, and diet-plus-exercise efforts have not led to durable results
- You want a more intensive intervention, but are not ready for surgery
- You are looking for a procedure with no external incisions
- You can commit to structured follow-up, nutrition changes, and long-term monitoring
It may be especially relevant for patients who are caught in the frustrating middle ground of obesity care: not responding well enough to lifestyle intervention, but not comfortable with, eligible for, or interested in surgery. Mayo Clinic specifically notes a BMI of 30 or higher as a possible threshold for ESG consideration when conservative methods have not worked.
Who may be a better fit for gastric sleeve surgery?
Gastric sleeve may be the stronger option when:
- A patient needs greater overall weight reduction
- Obesity-related complications are more severe
- A surgical bariatric team believes the metabolic benefit of surgery is more appropriate
- The patient is comfortable with a permanent anatomical change and the demands of surgical recovery
For some patients, especially those with higher BMI and significant metabolic disease, surgery remains the more powerful and better-studied intervention. This is why the right answer is not “Which one is better?” but “Which one fits the clinical picture, risk tolerance, and treatment goals?”
What about safety?
Both procedures require proper screening, experienced clinicians, and a structured aftercare plan.
Major medical centers and professional groups generally describe ESG as a safe and effective option when offered in an appropriate multidisciplinary setting.
The gastric sleeve has a much longer surgical track record. Still, because it is more invasive, it also comes with the broader risks that accompany bariatric operations that need professional medical management and counselling.
The more useful safety question for patients is not only “What can go wrong?” but also “How experienced is the treating team, and what follow-up support is in place?” Obesity treatment outcomes depend heavily on both.
Role of aftercare in both procedures

This is where patients often underestimate the process.
Neither ESG nor gastric sleeve works as a one-day fix. Both require post-procedure diet stages, behavior change, follow-up appointments, and monitoring for symptoms, nutrition, and long-term weight trajectory. In practice, the strongest programs treat the procedure as the beginning of a care pathway, not the whole pathway.
That is also why multidisciplinary care matters so much. The best outcomes are usually seen when the patient is supported by not just a proceduralist, but also dietitians, obesity-medicine clinicians, and nurses or coordinators who can help translate the procedure into daily life.
For patients exploring non-surgical intervention before considering surgery, programs that offer minimally invasive endoscopic sleeve gastroplasty alongside structured follow-up reflect the direction obesity care is moving: less about single interventions, more about integrated, physician-guided support.
Which option should patients choose?
The answer depends on what matters most.
If the priority is maximal weight loss and the patient is an appropriate surgical candidate, the gastric sleeve may remain the stronger option. If the priority is a less invasive, incision-free procedure with meaningful weight loss and shorter recovery, endoscopic sleeve gastroplasty may be a compelling choice.
The decision should ideally be made with a bariatric or obesity-care specialist who can assess BMI, metabolic health, prior weight-loss attempts, medication history, comorbidities, and personal preference. That kind of individualized conversation is more useful than comparing headline numbers alone.
Final Thoughts
Endoscopic sleeve gastroplasty and gastric sleeve surgery are not interchangeable, but they do belong in the same conversation. Both are designed to help patients with obesity achieve clinically meaningful weight loss. The main difference is that one does so through endoscopic reshaping of the stomach and the other through surgical removal of stomach tissue.
For patients who want more than lifestyle treatment but less than surgery, ESG has become an important bridge option. For others who need a stronger intervention and are comfortable with surgery, the gastric sleeve may still be the better fit.
Even after a procedure, nutrition and health habits continue to shape recovery, energy, and weight maintenance. The real progress in obesity care is not that there is one perfect treatment. It is that patients now have more than one evidence-based path forward.
References
Abu Dayyeh, B. K., et al. (2017).
- Endoscopic sleeve gastroplasty alters gastric physiology and induces loss of body weight in obese individuals.
- Clinical Gastroenterology and Hepatology
- DOI: 10.1016/j.cgh.2016.12.030
Lopez-Nava, G., et al. (2015).
- Endoscopic sleeve gastroplasty for obesity: a multicenter study.
- Endoscopy
- DOI: 10.1055/s-0034-1390773
Sharaiha, R. Z., et al. (2017).
- Five-year outcomes of endoscopic sleeve gastroplasty for the treatment of obesity.
- Gastrointestinal Endoscopy
- DOI: 10.1016/j.gie.2016.08.046
Hedjoudje, A., et al. (2020).
- Efficacy and safety of endoscopic sleeve gastroplasty: systematic review and meta-analysis.
- Clinical Gastroenterology and Hepatology
- DOI: 10.1016/j.cgh.2019.08.022
Schauer, P. R., et al. (2017).
- Bariatric surgery versus intensive medical therapy for diabetes — 5-year outcomes.
- New England Journal of Medicine
- DOI: 10.1056/NEJMoa1600869
Peterli, R., et al. (2018).
- Effect of laparoscopic sleeve gastrectomy vs laparoscopic Roux-en-Y gastric bypass on weight loss in patients with morbid obesity.
- JAMA
- DOI: 10.1001/jama.2018.20897
Arterburn, D. E., et al. (2020).
- Comparative effectiveness and safety of bariatric procedures for weight loss.
- Annals of Internal Medicine
- DOI: 10.7326/M19-3922
Kumar, N., et al. (2018).
- Endoscopic versus surgical therapies for obesity: a systematic review and meta-analysis.
- Gastrointestinal Endoscopy
- DOI: 10.1016/j.gie.2017.08.019
ASGE Bariatric Endoscopy Task Force (2021).
- Endoscopic bariatric therapies: ASGE guideline.
- Gastrointestinal Endoscopy
- DOI: 10.1016/j.gie.2020.10.013
Mechanick, J. I., et al. (2020).
- Clinical practice guidelines for perioperative nutrition, metabolic, and nonsurgical support of bariatric surgery patients.
- Endocrine Practice
- DOI: 10.4158/GL-2020-0406

