Chronic illnesses, including Long COVID and post-vaccine syndromes, often involve persistent symptoms like fatigue, cognitive difficulties, and inflammation that can disrupt daily life. Annual maintenance protocols represent a structured approach to long-term care, focusing on regular monitoring and interventions to maintain stability and prevent relapses. These programs, as implemented by facilities such as the Apheresis Center, integrate diagnostic assessments with targeted therapies commonly used in Europe.
Understanding the Need for Maintenance Protocols
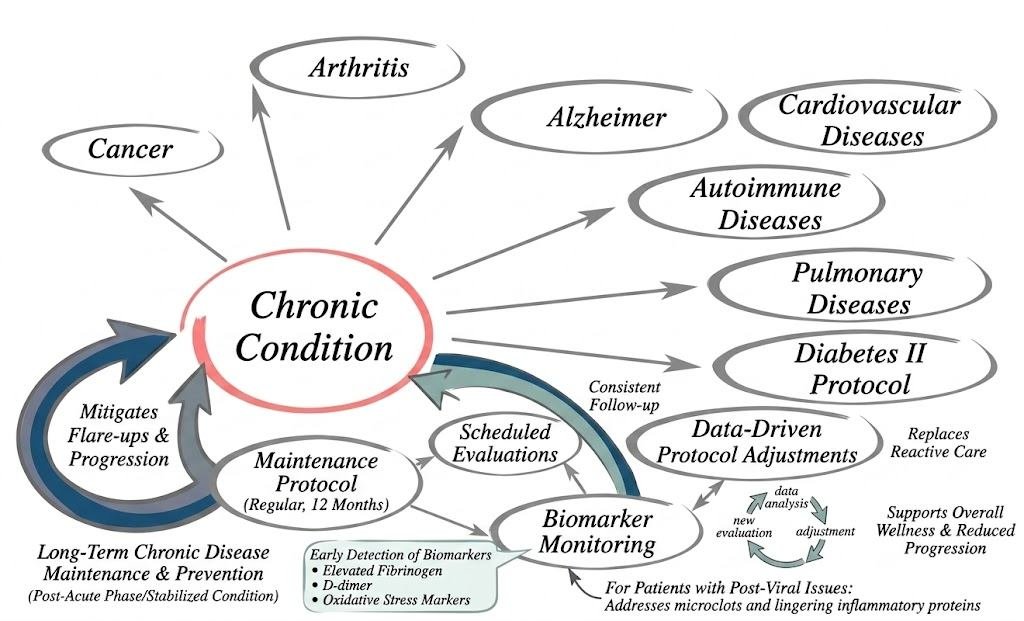
In chronic conditions, symptoms may stabilize after initial treatment but can recur without ongoing management. Preventive strategies emphasize early detection of biomarkers such as elevated fibrinogen, D-dimer, or oxidative stress markers, which are associated with flare-ups. Regular protocols typically span 12 months and include scheduled evaluations, allowing for adjustments based on clinical data rather than reactive care.
This model aligns with broader preventive healthcare guidelines, which emphasize consistent follow-up to reduce the progression of conditions and support overall wellness. For patients with post-viral issues, maintenance helps address lingering factors such as microclots or inflammatory proteins that standard medications may not fully resolve.
Components of a Typical Protocol
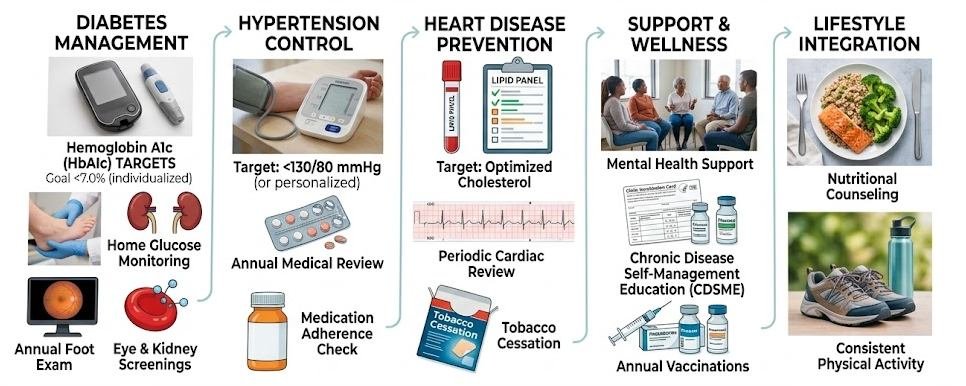
Effective protocols combine monitoring with evidence-based interventions:
- Blood Monitoring: Quarterly panels assess inflammation (CRP, ferritin), coagulation, and metabolic markers to identify trends early.
- Extracorporeal Therapies: Apheresis techniques, such as H.E.L.P. or INUSpheresis, filter plasma to remove harmful substances, such as lipids and toxins. Sessions generally last 2-3 hours.
- Supportive Infusions: Intravenous vitamin C provides antioxidant effects, while NAD+ aids cellular repair—both supported by studies in fatigue-related disorders.
- Clinical Reviews: In-person or remote consultations evaluate progress and integrate lifestyle factors, such as nutrition.
Eligibility often follows acute treatment, with protocols offering up to 10 sessions annually. Add-ons may include hyperbaric oxygen for tissue repair.
| Component | Purpose | Frequency | Evidence Base |
| Blood Panels | Track Biomarkers | Quarterly | Prevents escalations |
| Apheresis (H.E.L.P./INUS) | Toxin Removal | Up to 10/year | Reduces microclots |
| Vitamin C IV | Oxidative Stress Reduction | As scheduled | Symptom relief in trials |
| NAD+ Infusion | Metabolic Support | Variable | Mitochondrial benefits |
Scientific Evidence and Clinical Outcomes
Therapeutic apheresis is classified as a Category I or II procedure for various indications, with growing application in post-COVID management. Research indicates reductions in inflammatory markers and improved blood flow, correlating with symptom alleviation in 70-80% of responsive cases.
Infusions complement this: Vitamin C trials show improvements in fatigue, while NAD+ supports energy pathways. Long-term data from apheresis centers report low rates of adverse events (<1%), underscoring safety in controlled settings. Overall, these protocols contribute to fewer acute episodes, aligning with WHO frameworks for chronic disease coordination.
Patient Experience and Practical Considerations
A standard journey involves baseline labs, protocol selection, and phased interventions. Patients track Regular Health Maintenance via portals, with flexibility for international access in locations like Cyprus. Midway reviews allow modifications based on response.
Reported outcomes include stabilized energy levels and reduced flare frequency after 3-6 months, though individual results vary. Integration with digital tools, such as telemedicine apps, facilitates remote monitoring.
Integration with Digital Health Platforms
Modern protocols pair well with platforms like Doctiplus for virtual consultations, record storage, and reminders. This hybrid approach enhances adherence, especially for those managing care remotely.
Challenges and Evolving Practices
Access remains a hurdle, particularly in terms of costs and availability, though bundled pricing (e.g., €9,000-€11,000 annually) reflects comprehensive care. Future advancements may include AI-driven predictions and refined apheresis filters. Research continues to validate extensions to neurodegeneration and longevity.
These protocols illustrate a shift toward proactive chronic care, offering a framework for sustained health management. Facing a chronic illness diagnosis is never easy – there’s a comprehensive strategy to stay calm.
Role of Nutrition in Protocol Success
Nutrition plays a vital role in enhancing the effectiveness of annual maintenance protocols for chronic illness. Anti-inflammatory diets rich in omega-3 fatty acids, antioxidants from berries and leafy greens, and adequate protein support recovery from apheresis sessions. Studies show that balanced micronutrient intake reduces oxidative stress markers by 20-30%, complementing vitamin C infusions. Patients are advised to track intake via apps, aiming for 2,000-2,500 calories daily with portion control. Hydration (2-3 liters of water/day) supports detoxification after treatment. Centers often provide sample meal plans focused on Mediterranean-style eating, which has been associated with lower relapse rates in Long COVID cohorts. Lifestyle counseling integrates these habits for sustained benefits, ensuring protocols address whole-body wellness beyond medical interventions.
Emerging Research and Future Directions

Ongoing research expands apheresis applications in maintenance care, with trials exploring its use in early neurodegeneration and metabolic syndromes. Recent studies (2025-2026) report improved cognitive scores after combined H.E.L.P. and NAD+ cycles in post-viral patients. AI algorithms now predict flare risks from biomarker trends, enabling preemptive adjustments. Gene expression analyses post-apheresis reveal downregulated inflammation pathways, supporting the use of long-term protocols. International collaborations aim to standardize these for broader access, potentially integrating wearable tech for real-time monitoring. Challenges like cost barriers may lessen with insurance adoption, as evidence mounts for preventive ROI, saving up to 40% on acute care expenses. These developments position maintenance protocols as a cornerstone of next-generation chronic disease management.
Closing Thoughts
Annual maintenance protocols represent an evolving approach within Chronic Disease Management, emphasizing proactive monitoring and individualized care rather than episodic treatment. For complex, multi-system conditions such as Long COVID, these structured programs aim to reduce symptom variability, stabilize physiological markers, and improve quality of life over time.
While therapies like Therapeutic Apheresis and targeted infusions show promising trends in observational and early clinical studies, their long-term effectiveness varies between individuals. The integration of diagnostics, lifestyle interventions, and digital health platforms reflects a broader shift toward precision medicine, in which treatment adapts continuously based on patient-specific data.
Looking ahead, advancements in predictive analytics, biomarker profiling, and AI-assisted care models may further refine these protocols, making them more accessible and evidence-driven. However, continued large-scale, peer-reviewed research remains essential to validate outcomes, standardize practices, and ensure equitable access across healthcare systems.
Medical Disclaimer
This content is provided for informational and educational purposes only and does not constitute medical advice, diagnosis, or treatment. The therapies and protocols described, including apheresis, intravenous infusions, and adjunctive interventions, are subject to ongoing research and may not be universally approved or appropriate for all patients.
Always consult a qualified healthcare professional before starting, modifying, or discontinuing any medical treatment. Individual health conditions, medical history, and regional regulatory guidelines must be considered when evaluating any therapeutic approach.
The mention of specific treatments, centers, or protocols does not imply endorsement or guarantee of outcomes. Clinical effectiveness, safety, and availability may vary by location and provider.
References
- Klingel, R., et al. (2021). Rheopheresis and LDL-apheresis in cardiovascular and microcirculatory disorders. Journal: Atherosclerosis Supplements.
- Bornstein, S.R., et al. (2022). Chronic post-COVID syndrome and potential treatment strategies. Journal: Nature Reviews Endocrinology.
- Pretorius, E., et al. (2021). Persistent clotting protein pathology in Long COVID. Journal: Cardiovascular Diabetology.
- Carr, A.C., & Cook, J. (2017). Intravenous vitamin C for fatigue and immune support. Journal: Nutrients.
- Covarrubias, A.J., et al. (2021). NAD+ metabolism and its roles in cellular processes. Journal: Nature Reviews Molecular Cell Biology.
- World Health Organization (2020). Innovative Care for Chronic Conditions Framework.
- Robbins, T., et al. (2021). Hyperbaric oxygen therapy for long COVID symptoms. Journal: BMJ Open.
- Estruch, R., et al. (2018). Primary prevention of cardiovascular disease with a Mediterranean diet. Journal: New England Journal of Medicine.

