Beginning in the early to mid-40s, many adults start having problems seeing clearly at close distances, making it one of the most common health changes among people between the ages of 41 and 60. By the time the symptoms become disruptive enough to act on, the window for low-intervention management has often already narrowed.
The good news is that most age-related eye conditions are either manageable or preventable from becoming serious when caught early. This article covers what is actually happening to your eyes after 40, which conditions are worth watching for, and what to do about each of them.
Why Your Eyes Change After 40

The eye is a remarkably precise organ, and like all precision systems, it becomes more sensitive to wear over time.
The lens, responsible for focusing light onto the retina, gradually loses its elasticity. The ciliary muscles that control the lens also weaken, reducing the eye’s ability to shift focus quickly between near and far distances. At the same time, the vitreous humor, the gel-like substance inside the eye, begins to shrink and pull slightly away from the retina. This is when many people first notice floaters, those specks or strings that drift across the visual field. For most people, floaters are benign. In some cases, however, they signal something more serious.
These biological shifts are universal. They affect virtually everyone, regardless of whether they wore corrective lenses earlier in life. What varies is the pace and the degree, and that is where lifestyle, genetics, and early intervention make a real difference.
Conditions Most Likely to Emerge in Your 40s
Presbyopia
Presbyopia is the clinical term for the gradual loss of near-focusing ability. It is not a disease or a disorder. It is simply the result of a lens that has become less flexible over decades of use. The name comes from the Greek for “old eye,” which is somewhat misleading given that it typically begins in a person’s early to mid-40s.
Common signs include holding books or phones further away to see them clearly, needing brighter light to read comfortably, and experiencing mild eye fatigue or headaches after close-up work.
For most adults, the first and most practical response is a pair of progressive reading glasses. The key point is not to ignore the symptoms or push through the strain. Presbyopia is entirely manageable, and the sooner it is addressed, the more comfortable daily life becomes.
Dry Eye Disease
The tear film that keeps the eye surface lubricated becomes less stable with age. For many people in their 40s and beyond, this manifests as persistent dryness, a burning or gritty sensation, intermittent blurry vision, or paradoxically, excessive tearing. It is significantly more common in women, particularly around perimenopause, when hormonal changes affect tear production.
Dry eye is frequently underdiagnosed because it is easy to attribute symptoms to screen use or a dry environment. Both can contribute, but they are not always the root cause.
How to manage it: Preservative-free artificial tear drops are the standard first-line option and provide meaningful relief for mild cases. For moderate to severe dry eye, an eye care professional may recommend prescription drops such as cyclosporine, punctal plugs to reduce tear drainage, or omega-3 supplementation, which has some evidence behind it for improving tear quality. Reducing screen time, using a humidifier, and staying well hydrated also help manage symptoms day to day.
Glaucoma
Glaucoma is a group of conditions that damage the optic nerve, most commonly as a result of elevated pressure inside the eye. It progresses silently in most cases, producing no pain and no noticeable vision changes in its early stages. By the time peripheral vision begins to close in, significant and irreversible damage has already occurred. This is precisely why it is among the leading causes of preventable blindness worldwide.
The risk increases markedly after 40, particularly in people with a family history of glaucoma, those of African or Hispanic descent, and individuals with diabetes or hypertension.
How to manage it: There is no cure for glaucoma, but progression can be slowed or halted with consistent treatment. Prescription eye drops that reduce intraocular pressure are the most common approach. Laser therapy and surgical procedures are options when drops are insufficient. The critical point is that treatment only works if the condition is detected early, which makes regular comprehensive eye exams non-negotiable for anyone in a higher-risk group.
Cataracts
A cataract forms when proteins in the lens begin to clump together, gradually clouding what was once a clear structure. Most people develop some degree of cataract formation after 40, though significant visual impairment typically develops in the 60s and beyond. Early signs include increased sensitivity to glare, colors that appear duller than they used to, and a slight haze over the visual field, particularly in bright light or at night.
How to manage it: When cataracts progress to the point where they meaningfully interfere with daily life, surgery is the definitive solution. Cataract surgery involves replacing the clouded natural lens with a clear artificial one and is among the safest and most successful procedures performed today.
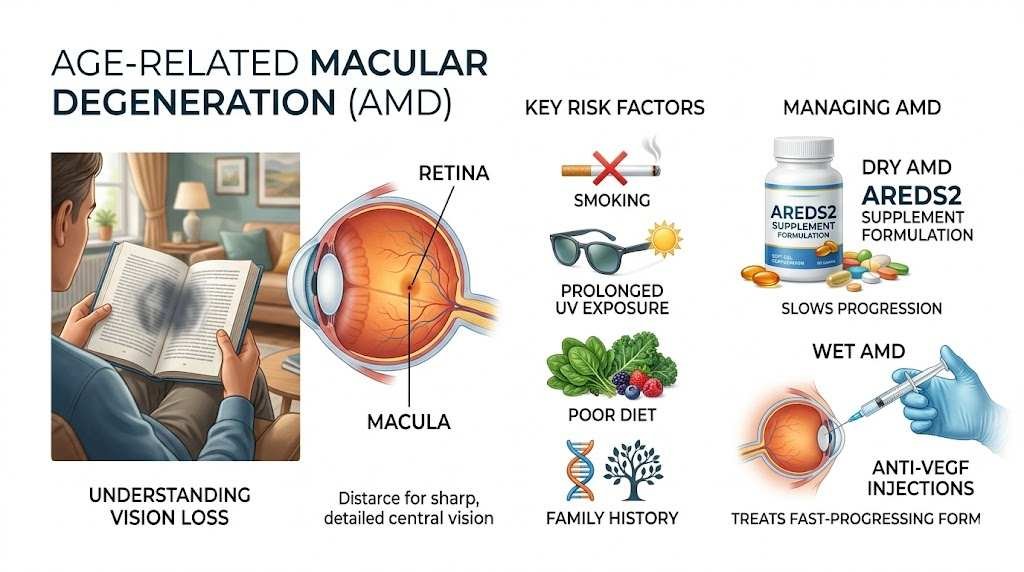
Age-Related Macular Degeneration (AMD)
The macula is the small central region of the retina responsible for sharp, detailed vision. Tasks like reading, recognizing faces, and driving all depend on it. As the macula deteriorates, central vision becomes blurred or distorted, while peripheral vision often remains intact. AMD ranges from early, where there may be no symptoms at all, to advanced, where central vision loss can be severe.
Smoking, prolonged UV exposure, poor diet, and a family history of the condition are known risk factors. AMD does not always progress to serious vision loss, but for those with advanced forms, the consequences are significant.
How to manage it: There is no cure for AMD, but management varies by type. Dry AMD, the more common form, can be slowed in higher-risk individuals with the AREDS2 supplement formulation, a specific combination of vitamins and minerals shown in clinical trials to reduce the risk of progression. Wet AMD, a less common but faster-progressing form, is treated with anti-VEGF injections administered by a retinal specialist, which can preserve or, in some cases, improve vision when started early. Low-vision aids and rehabilitation services are available for those who experience significant loss.
Lifestyle Habits That Support Eye Health After 40
No supplement or daily habit will reverse presbyopia or eliminate the risk of cataracts. But there is solid evidence that certain choices reduce risk and slow the progression of several age-related conditions.
- Protect your eyes from UV exposure. Cumulative sun exposure contributes to both cataract development and macular damage. Wearing sunglasses that block 100 percent of UVA and UVB radiation is a simple and highly effective protective measure that many people still overlook.
- Eat for your retinas. Leafy greens, oily fish, eggs, and citrus fruits provide lutein, zeaxanthin, omega-3 fatty acids, and vitamins C and E, all of which support retinal health. A diet consistently rich in these nutrients is associated with lower AMD risk.
- Manage systemic health conditions. Diabetes and hypertension both affect the blood vessels supplying the retina. Controlling blood sugar and blood pressure directly reduces the risk of diabetic retinopathy and hypertensive retinopathy, two serious vision-threatening conditions that often develop without warning.
- Be deliberate about screen habits. The 20-20-20 rule, looking at something 20 feet away for 20 seconds every 20 minutes, remains a widely recommended strategy for reducing digital eye strain. It does not undo underlying conditions, but it reduces the compounding effect of prolonged close focus on an eye system that is already adapting to age-related changes.
Closing
Turning 40 does not mean your vision is in freefall. Most of what happens to your eyes during this period is predictable, well-understood, and manageable with the right combination of professional care and informed habits.
The conditions covered here range from minor inconveniences to serious risks, but they share one thing in common: outcomes are significantly better when they are caught early. That starts with a comprehensive eye exam and a willingness to take small changes seriously rather than adapting around them.
Disclaimer
This article is intended for informational and educational purposes only and should not be considered medical advice, diagnosis, or treatment recommendations. Eye conditions and vision changes can vary significantly between individuals. Readers should consult a qualified ophthalmologist, optometrist, or healthcare provider for personalized evaluation and guidance regarding any symptoms or concerns related to eye health. Early detection and professional assessment are essential for preventing potential vision complications. Never ignore sudden vision loss, flashes of light, severe eye pain, or other urgent symptoms, as these may require immediate medical attention.
References
- Charman WN. The eye in focus: accommodation and presbyopia. Clin Exp Optom. 2008;91(3):207-225. DOI: 10.1111/j.1444-0938.2008.00218.x
- Stapleton F, Alves M, Bunya VY, et al. TFOS DEWS II Epidemiology Report. Ocul Surf. 2017;15(3):334-365. DOI: 10.1016/j.jtos.2017.05.003
- Tham YC, Li X, Wong TY, et al. Global prevalence of glaucoma and projections of glaucoma burden through 2040. Ophthalmology. 2014;121(11):2081-2090. DOI: 10.1016/j.ophtha.2014.05.013
- Asbell PA, Dualan I, Mindel J, et al. Age-related cataract. Lancet. 2005;365(9459):599-609. DOI: 10.1016/S0140-6736(05)17911-2
- Wong WL, Su X, Li X, et al. Global prevalence of age-related macular degeneration and disease burden projection for 2020 and 2040. Lancet Glob Health. 2014;2(2):e106-e116. DOI: 10.1016/S2214-109X(13)70145-1
- Age-Related Eye Disease Study 2 (AREDS2) Research Group. Lutein + Zeaxanthin and Omega-3 Fatty Acids for Age-Related Macular Degeneration. JAMA. 2013;309(19):2005-2015. DOI: 10.1001/jama.2013.4997
- Rosenfield M. Computer vision syndrome: a review of ocular causes and potential treatments. Ophthalmic Physiol Opt. 2011;31(5):502-515. DOI: 10.1111/j.1475-1313.2011.00834